Unicompartmental Knee Replacement
Partial knee replacement — preserving your healthy knee while replacing only the damaged compartment for faster recovery and more natural function
Introduction
Unicompartmental knee replacement (UKR), also known as partial knee replacement, is a highly effective, minimally invasive procedure for patients whose arthritis is confined to a single compartment of the knee. Unlike total knee replacement, which resurfaces the entire joint, UKR preserves the healthy bone, cartilage, and ligaments — resulting in a more natural-feeling knee, faster recovery, and excellent long-term results.
At JointClinics, we use the latest evidence-based techniques and implant technology, including robotic-assisted surgery, to deliver outstanding outcomes. Our surgeons have extensive experience in partial knee replacement and will guide you through every step of your journey. Research shows that up to 50% of patients requiring knee replacement may be eligible for this less invasive option.
Understanding Your Knee
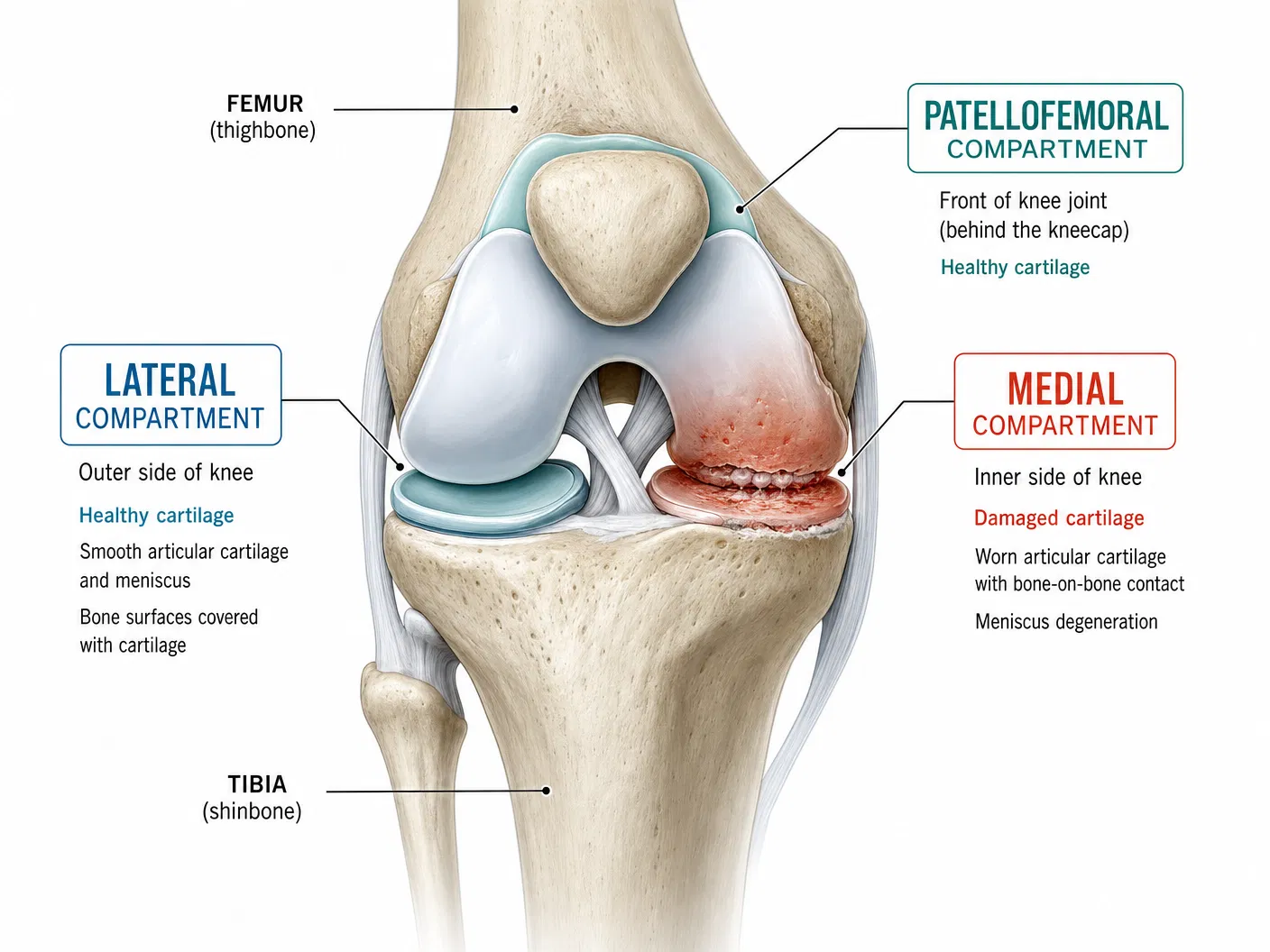
The knee is the largest and one of the most complex joints in the body. It is formed by three bones: the femur (thighbone), the tibia (shinbone), and the patella (kneecap). These bones are covered with a smooth layer of articular cartilage that allows pain-free movement.
The knee is divided into three distinct compartments. In a healthy knee, all three work together to provide smooth, pain-free movement. However, osteoarthritis can sometimes affect just one compartment — most commonly the medial (inner) compartment — while the other compartments remain healthy. This pattern is called anteromedial osteoarthritis (AMOA) and is the ideal indication for unicompartmental knee replacement.
| Compartment | Location | Description |
|---|---|---|
| Medial | Inner side of the knee | Between the inner surfaces of the femur and tibia |
| Lateral | Outer side of the knee | Between the outer surfaces of the femur and tibia |
| Patellofemoral | Front of the knee | Between the kneecap and the front of the femur |
What Is Unicompartmental Knee Replacement?
Unicompartmental knee replacement is a surgical procedure in which only the damaged compartment of the knee is replaced with an artificial implant. The healthy cartilage, bone, and all of the ligaments in the remaining compartments are preserved. Because only one compartment is resurfaced, the surgery is performed through a smaller incision (typically 7–10 cm) compared to total knee replacement (15–20 cm).
This minimally invasive approach causes less disruption to the surrounding muscles and soft tissues, which is a key reason for the faster recovery. The concept was first developed in the 1950s, and modern designs have been in use since the early 1970s. The Oxford Unicompartmental Knee, introduced in the 1980s, remains one of the most widely used and extensively studied partial knee implants worldwide, with 10-year survival rates of 96% in specialist centres.
Are You a Suitable Candidate?
Not everyone with knee arthritis is suitable for a partial knee replacement. Your surgeon will perform a thorough assessment. Modern evidence-based criteria (Oxford indications) suggest you may be a good candidate if you have:
Bone-on-bone arthritis in one compartment (confirmed on X-ray)
Intact, functioning anterior cruciate ligament (ACL)
Stable medial collateral ligament (MCL)
Full-thickness cartilage in the lateral compartment
A correctable deformity (leg straightens with stress)
Modern research has shown that age, body weight, activity level, and the presence of patellofemoral changes are NOT contraindications to UKR when performed by an experienced surgeon using appropriate implants.
Contraindications
| Contraindication | Reason |
|---|---|
| Inflammatory arthritis (e.g., rheumatoid) | Affects all compartments simultaneously |
| Absent or torn ACL | Leads to abnormal knee mechanics and implant failure |
| Fixed flexion contracture >15° | Indicates more widespread joint disease |
| Significant ligament instability | Cannot maintain normal joint alignment |
| Active infection | Risk of implant infection |
| Arthritis in multiple compartments | Requires total knee replacement instead |
UKR vs Total Knee Replacement
Understanding the differences between partial and total knee replacement can help you appreciate why your surgeon may recommend one procedure over the other. Research from the UK National Joint Registry involving over 100,000 knee replacements demonstrates that major complications occur between a quarter and a half times less frequently with UKR compared to TKR.
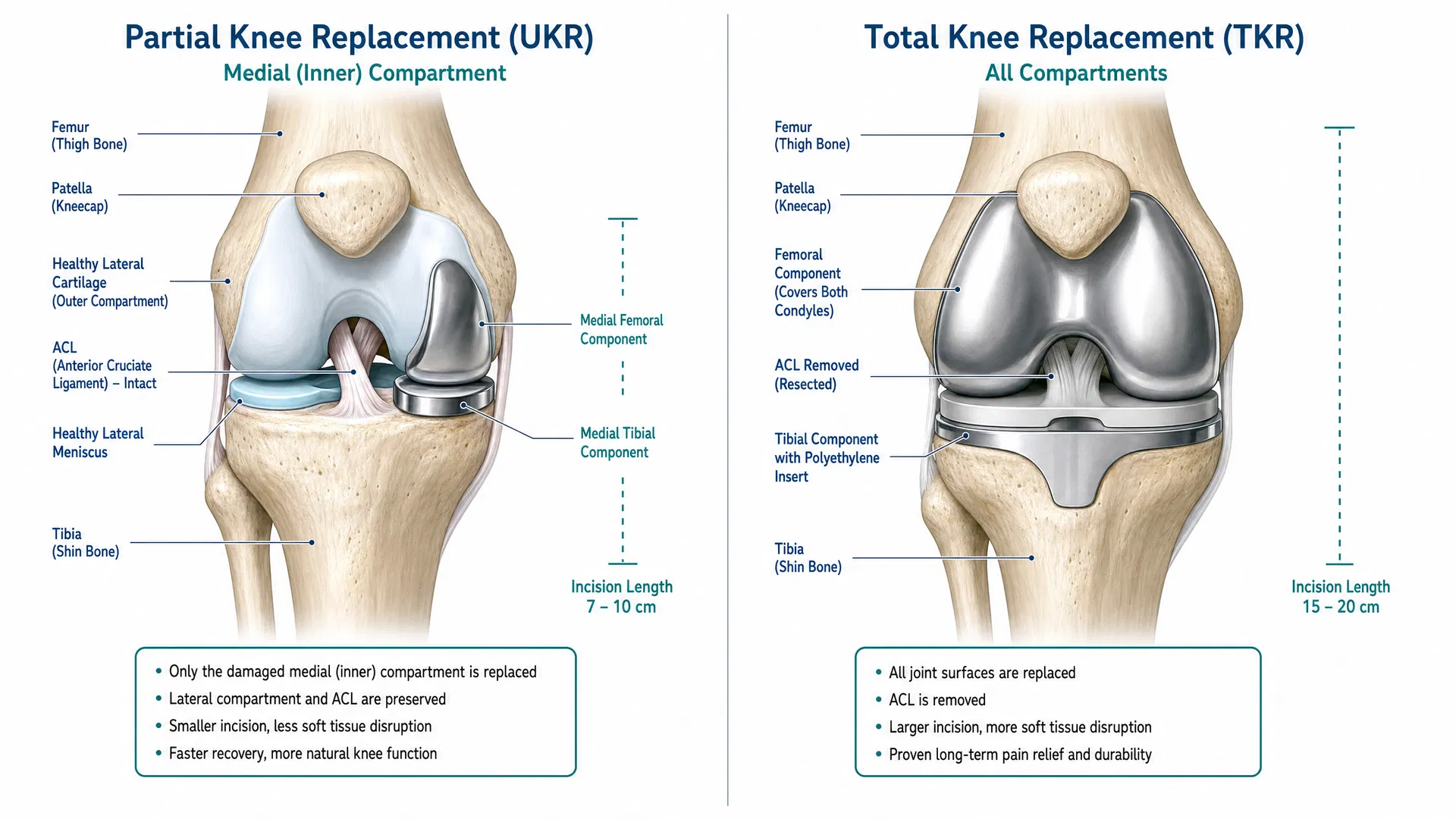
| Feature | UKR (Partial) | TKR (Total) |
|---|---|---|
| What is replaced | One compartment only | All three compartments |
| Incision size | 7–10 cm | 15–20 cm |
| Bone removed | Minimal (3–4 mm) | Substantial |
| Ligaments | All preserved (including ACL) | ACL removed |
| Hospital stay | Day-case or 1 night | 1–3 nights |
| Return to driving | 2–4 weeks | 4–6 weeks |
| Full recovery | 6–12 weeks | 3–6 months |
| Blood loss | Minimal | Moderate |
| Infection risk | Lower (0.2–0.5%) | Higher (0.5–1.5%) |
| Range of motion | Average 130° | Average 115–120° |
| "Natural" feel | More natural | Less natural |
| 10-year survival | 93–97% | 95–98% |
| Revision rate | Higher | Lower |
Your New Knee — Implant Components
A unicompartmental knee implant consists of three main components that work together to recreate the smooth, pain-free movement of a healthy joint surface.
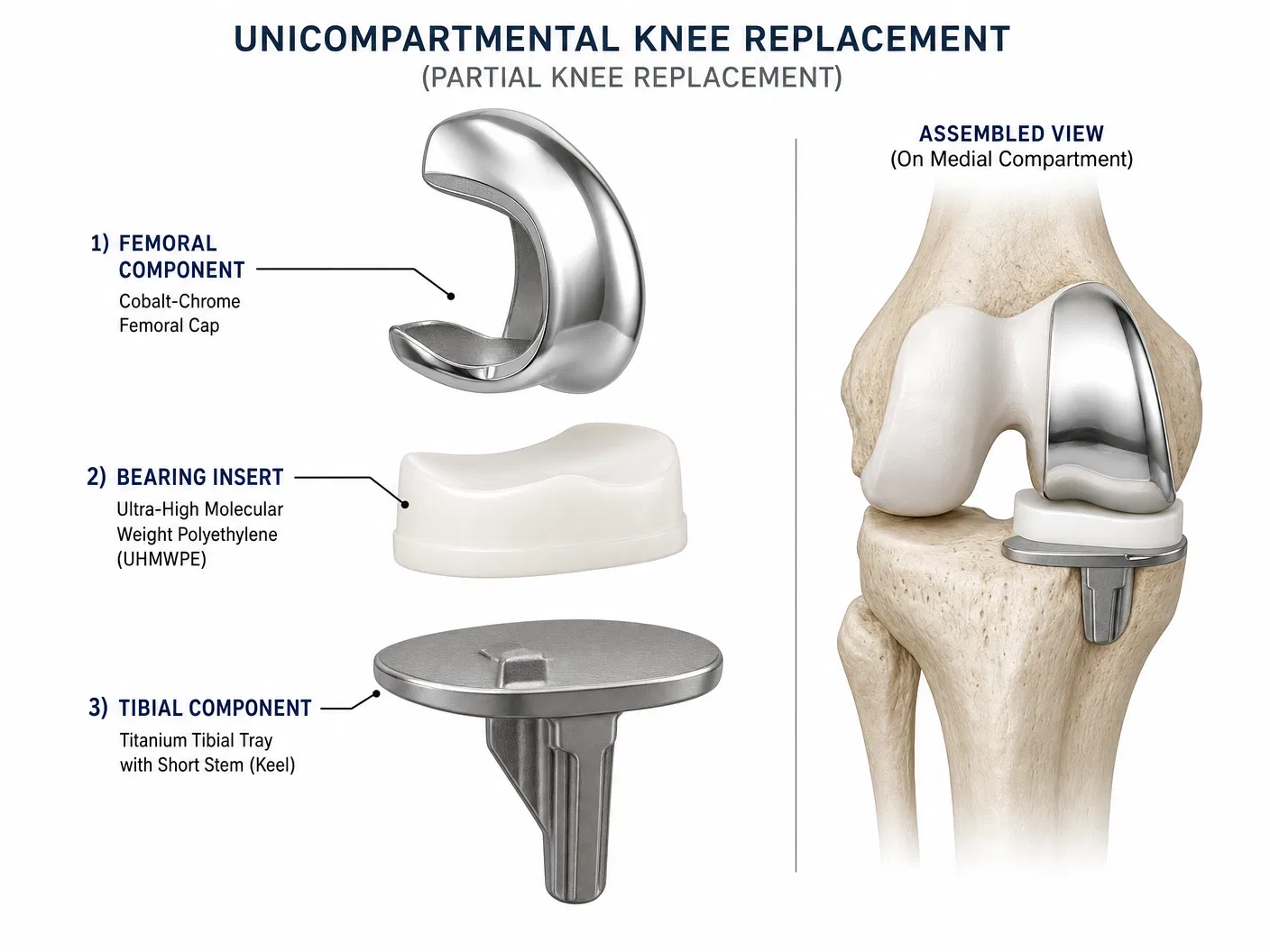
| Component | Material | Function |
|---|---|---|
| Femoral component | Cobalt-chrome alloy | Caps the end of the thighbone in the affected compartment |
| Tibial component | Cobalt-chrome or titanium alloy | Sits on top of the shinbone, providing a flat platform |
| Bearing insert | Ultra-high molecular weight polyethylene | Sits between the metal components, allowing smooth gliding |
Fixed Bearing vs Mobile Bearing
Fixed bearing — The plastic insert is locked to the tibial component and does not move. Mobile bearing — The plastic insert is free to move (rotate and slide) on the tibial component, pioneered by the Oxford knee, aiming to reduce wear and distribute forces more evenly. Both designs demonstrate excellent long-term results.
Cemented vs Cementless Fixation
Implants can be fixed using bone cement or press-fit without cement, relying on bone growing onto the implant surface. Recent evidence from the New Zealand Joint Registry shows the revision rate of cementless UKR is approximately half that of cemented UKR, with advantages including fewer radiolucent lines and faster surgical time.
The Surgical Procedure
UKR is most commonly performed under spinal anaesthesia combined with sedation. The procedure typically takes 45–60 minutes — significantly shorter than total knee replacement.
Incision
A small incision (7–10 cm) is made on the inner side of the knee, following natural skin creases.
Exposure
The joint is opened through a minimally invasive approach that avoids cutting through the quadriceps muscle. The kneecap is gently moved aside without dislocating it.
Assessment
The surgeon confirms arthritis is confined to one compartment and the ACL is intact. Other compartments are inspected.
Bone Preparation
Using precision cutting guides (or robotic assistance), a thin layer of damaged bone (only 3–4 mm) is removed — far less than in total knee replacement.
Trial Components
Trial implants are inserted to check fit, alignment, and balance through a full range of motion.
Final Implants
Definitive implants are cemented or press-fit into position. The bearing insert is placed between the metal components.
Closure
The joint capsule and skin are closed in layers. A waterproof dressing is applied.
Robotic-Assisted Surgery
At JointClinics, we offer robotic-assisted UKR providing 3D planning and real-time intraoperative guidance. This achieves implant positioning accuracy within 1° of the planned alignment and soft tissue balancing to within 1 mm of the target, with haptic boundaries protecting healthy bone and ligaments.
Preparing for Surgery (Prehabilitation)
Preparing your body before surgery — known as prehabilitation — can significantly improve your recovery. We recommend starting 4–6 weeks before your operation.
| Exercise | Purpose | Frequency |
|---|---|---|
| Straight leg raises | Strengthen quadriceps | 3 sets of 10, twice daily |
| Heel slides | Maintain knee flexion | 3 sets of 10, twice daily |
| Static quads | Activate thigh muscles | 10-sec holds ×10, twice daily |
| Ankle pumps | Improve circulation | 20 reps, 4 times daily |
| Walking | General fitness | 20–30 minutes daily |
| Stationary cycling | Low-impact conditioning | 15–20 mins, 3× weekly |
Your Hospital Stay and Discharge
One of the major advantages of UKR over total knee replacement is the shorter hospital stay. Many patients are discharged on the same day as surgery (day-case) or after a single overnight stay. Most patients stand and take their first steps within 2–4 hours of surgery.
Discharge Criteria
Walk safely with crutches on a flat surface
Get in and out of bed independently
Climb a few stairs (if needed at home)
Manage pain with oral medications
Pass urine normally
Understand exercise programme and follow-up plan
Pain Management After Surgery
We use a multimodal approach combining different types of pain relief to minimise discomfort while reducing the need for strong opioids.
| Medication | Type | Duration |
|---|---|---|
| Paracetamol | Simple analgesic | 4–6 weeks |
| Ibuprofen/Naproxen | Anti-inflammatory (NSAID) | 2–4 weeks |
| Codeine/Tramadol | Weak opioid | 1–2 weeks (reduce quickly) |
| Local anaesthetic injection | Nerve block | 12–24 hours |
| Ice therapy | Non-pharmacological | As needed, first 2 weeks |
Rehabilitation Programme
Recovery after UKR is significantly faster than after total knee replacement. Most patients notice a dramatic improvement within the first 6 weeks.
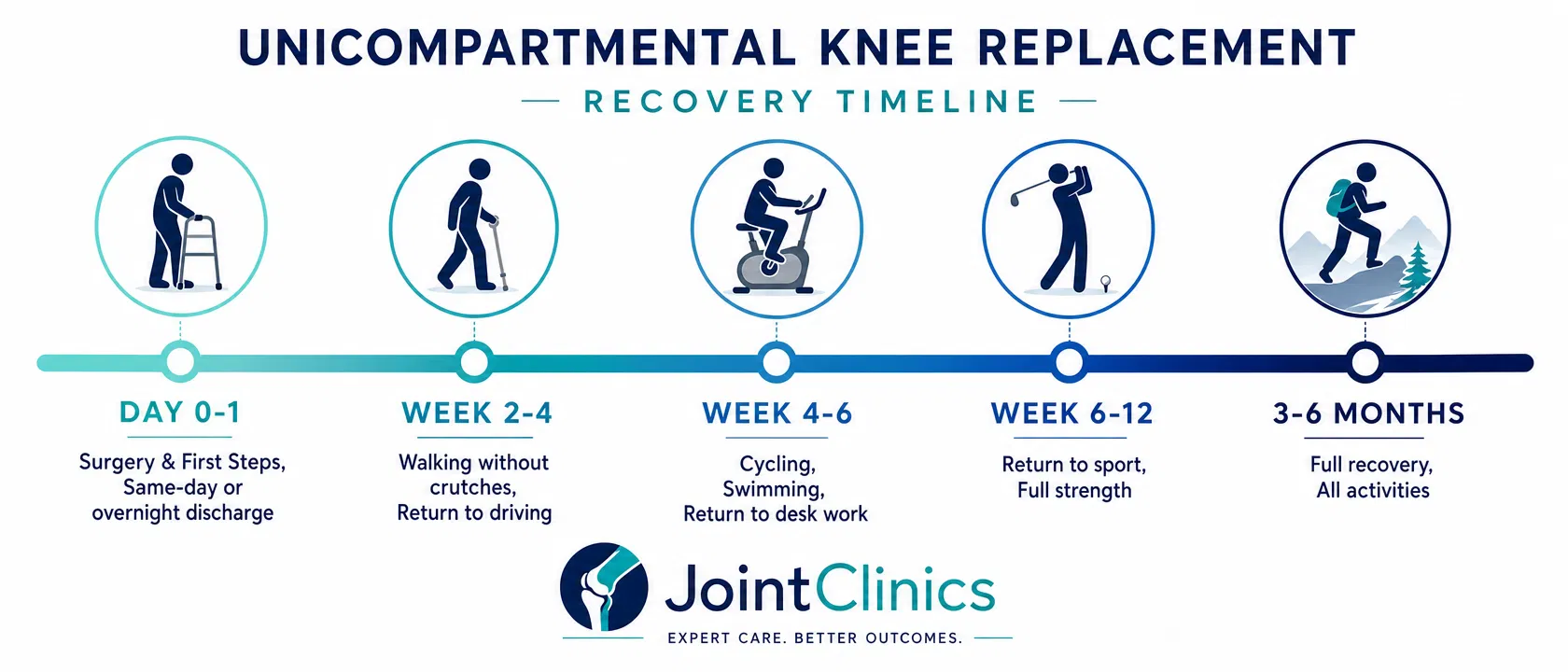
Phase 1: Immediate Post-Operative (Days 0–14)
Goals: Control swelling, restore knee extension, begin flexion, walk safely with crutches
| Exercise | Description | Repetitions |
|---|---|---|
| Ankle pumps | Circle and pump ankles up and down | 20 reps, every hour |
| Static quadriceps | Tighten thigh muscle, push knee flat | 10×10-sec holds, 3× daily |
| Heel slides | Slide heel towards buttock, bending knee | 10 reps, 3× daily |
| Straight leg raise | Lift leg 15 cm off bed, knee straight | 10 reps, 3× daily |
| Knee extension stretch | Place heel on rolled towel, let knee straighten | 5 minutes, 4× daily |
Phase 2: Early Recovery (Weeks 2–6)
Goals: Wean off crutches, restore normal gait, achieve full range of motion
| Exercise | Description | Repetitions |
|---|---|---|
| Stationary cycling | Low resistance, full revolutions | 10–15 minutes daily |
| Step-ups | Step up onto a low step (10–15 cm) | 10 reps each leg, 3× daily |
| Wall squats | Slide down wall to 45°, hold 5 seconds | 10 reps, 3× daily |
| Calf raises | Rise onto tiptoes, hold 3 seconds | 10 reps, 3× daily |
| Balance exercises | Stand on operated leg, 30 seconds | 5 reps, 3× daily |
Phase 3: Strengthening (Weeks 6–12)
Goals: Build muscle strength, improve endurance, return to recreational activities
| Exercise | Description | Repetitions |
|---|---|---|
| Leg press | Light-moderate resistance | 3×12 reps, 3× weekly |
| Lunges | Forward and lateral lunges | 3×10 reps, 3× weekly |
| Swimming/aqua jogging | Low-impact cardiovascular fitness | 20–30 mins, 3× weekly |
| Outdoor cycling | Gradually increase distance | 20–30 mins, 3× weekly |
| Single-leg balance | Eyes closed, unstable surface | 30 sec ×5, daily |
Phase 4: Return to Full Activity (3–6 Months)
Continue strengthening exercises 2–3 times weekly. Gradually return to higher-impact activities as tolerated. Maintain healthy weight and regular exercise for implant longevity. Annual review with your surgeon or physiotherapist.
Returning to Activities
One of the great advantages of UKR is the ability to return to a wide range of activities, including many sports. The following table provides general guidance.
| Activity | Timeline | Notes |
|---|---|---|
| Driving (automatic) | 2–3 weeks | When safe to perform emergency stop |
| Desk work | 2–4 weeks | May need breaks to elevate leg |
| Light housework | 2–3 weeks | Avoid heavy lifting initially |
| Golf | 6–8 weeks | Start with putting and chipping |
| Swimming | 4–6 weeks | Once wound fully healed |
| Cycling | 4–6 weeks | Stationary bike earlier |
| Doubles tennis | 8–12 weeks | Avoid aggressive lunging initially |
| Hiking | 8–12 weeks | Start with flat terrain |
| Manual work | 8–12 weeks | Depends on physical demands |
| Skiing | 3–6 months | Good technique required |
| Running (jogging) | 3–6 months | Discuss with surgeon |
Risks and Complications
All surgery carries some risk. UKR is a safe procedure with a low complication rate — significantly lower than total knee replacement for most complications.
Common (1 in 10 to 1 in 100)
Uncommon (1 in 100 to 1 in 1000)
Rare (Less than 1 in 1000)
Revision to TKR: If the implant fails or arthritis progresses, UKR can be converted to a total knee replacement. Because healthy bone and ligaments are preserved, revision is generally straightforward with results comparable to a primary TKR.
Long-Term Outcomes and Implant Survival
Unicompartmental knee replacement has an excellent track record when performed on appropriate patients by experienced surgeons. Over 90% of patients report good or excellent outcomes, and many describe their knee as feeling "forgotten."
| Source | Implant | 10-Year Survival |
|---|---|---|
| Pandit et al. (2013) | Oxford Phase 3 | 96% |
| Mohammad et al. (systematic review) | Oxford UKR | 93% |
| Cementless Oxford (specialist centre) | Oxford Cementless | 97.5% |
| UK National Joint Registry | All UKR | 88% |
Frequently Asked Questions
How long does the operation take?
The surgery typically takes 45–60 minutes. You will be in the operating theatre for approximately 90 minutes in total, including anaesthetic preparation.
Will I be awake during surgery?
Most patients have a spinal anaesthetic with sedation — numb from the waist down and relaxed but not fully asleep. A general anaesthetic is also available if you prefer.
How long will I stay in hospital?
Most patients go home on the same day as surgery or after one night. This is significantly shorter than total knee replacement.
When can I drive?
Most patients can drive within 2–4 weeks, once they can safely perform an emergency stop. For left knee surgery with an automatic car, this may be as early as 2 weeks.
When can I return to work?
Desk work: 2–4 weeks. Light physical work: 4–6 weeks. Heavy manual work: 8–12 weeks.
Will my knee feel normal?
Many patients report that their UKR feels more natural than a total knee replacement because the healthy ligaments and cartilage are preserved. Some describe 'forgetting' they have an artificial knee.
How long will the implant last?
Modern UKR implants have a 10-year survival rate of 93–97% in specialist centres. Many last 15–20 years or longer.
Can I kneel after surgery?
Yes, most patients can kneel after UKR, although it may feel uncomfortable initially. Using a cushion or kneeling pad helps.
Will I need the other side replaced later?
Possibly, if arthritis progresses. However, many patients never require further surgery. Converting UKR to TKR is straightforward with good outcomes.
Is robotic surgery better?
Robotic-assisted surgery improves accuracy and consistency of implant positioning. Early results are promising, but long-term comparative data is still being collected.
Warning Signs — When to Seek Help
Contact JointClinics or attend your nearest Emergency Department immediately if you experience:
Possible Infection
High fever (>38.5°C) with wound redness
Wound breakdown or pus discharge
Increasing redness, warmth, or swelling
Possible Blood Clot (DVT/PE)
Sudden severe calf pain or swelling
Sudden breathlessness or chest pain
Sudden inability to weight-bear
Emergency Contact: 07553 209288 | If chest pain or breathlessness — call 999 immediately.
References
- Campi S, Tibrewal S, Cuthbert R, Tibrewal SB. Unicompartmental knee replacement — Current perspectives. J Clin Orthop Trauma. 2017;9(1):17–23.
- Pandit H, Hamilton TW, Jenkins C, et al. The clinical outcome of minimally invasive Phase 3 Oxford unicompartmental knee arthroplasty: a 15-year follow-up of 1000 UKAs. Bone Joint J. 2015;97-B(11):1493–1500.
- Mohammad HR, Strickland L, Hamilton TW, Murray DW. Long-term outcomes of over 8,000 medial Oxford Phase 3 Unicompartmental Knees. Acta Orthop. 2018;89(1):101–107.
- Liddle AD, Judge A, Pandit H, Murray DW. Adverse outcomes after total and unicompartmental knee replacement in 101,330 matched patients. Lancet. 2014;384(9952):1437–1445.
- Wilson HA, Middleton R, Abram SGF, et al. Patient relevant outcomes of unicompartmental versus total knee replacement: systematic review and meta-analysis. BMJ. 2019;364:l352.
- Murray DW, Parkinson RW. Usage of unicompartmental knee arthroplasty. Bone Joint J. 2018;100-B(4):432–435.
- Goodfellow JW, Tibrewal SB, Sherman KP, O'Connor JJ. Unicompartmental Oxford Meniscal Knee Arthroplasty. J Arthroplasty. 1987;2(1):1–9.
- National Joint Registry for England, Wales, Northern Ireland and the Isle of Man. 20th Annual Report 2023.
- Price AJ, Alvand A, Troelsen A, et al. Knee replacement. Lancet. 2018;392(10158):1672–1682.
- Li J, et al. Enhanced recovery after surgery (ERAS) protocol in geriatric patients undergoing unicompartmental knee arthroplasty. 2023.