Total Knee Replacement Surgery
Including the JointClinics Fast Recovery Programme — evidence-based enhanced recovery for faster return to normal life
Introduction
Total knee replacement (also known as total knee arthroplasty, or TKA) is one of the most successful operations in modern medicine. It reliably reduces pain, restores function, and improves quality of life for patients with severe knee arthritis. Over 100,000 knee replacements are performed each year in the United Kingdom, and the vast majority of patients report significant improvement in their symptoms.
At JointClinics, we use an Enhanced Recovery After Surgery (ERAS) programme — our "Fast Recovery Programme" — which is designed to get you moving quickly, reduce your hospital stay, and help you return to your normal activities as soon as safely possible. Research consistently demonstrates that patients who follow enhanced recovery protocols experience fewer complications, shorter hospital stays, and better functional outcomes compared with traditional care pathways.
Understanding Your Knee
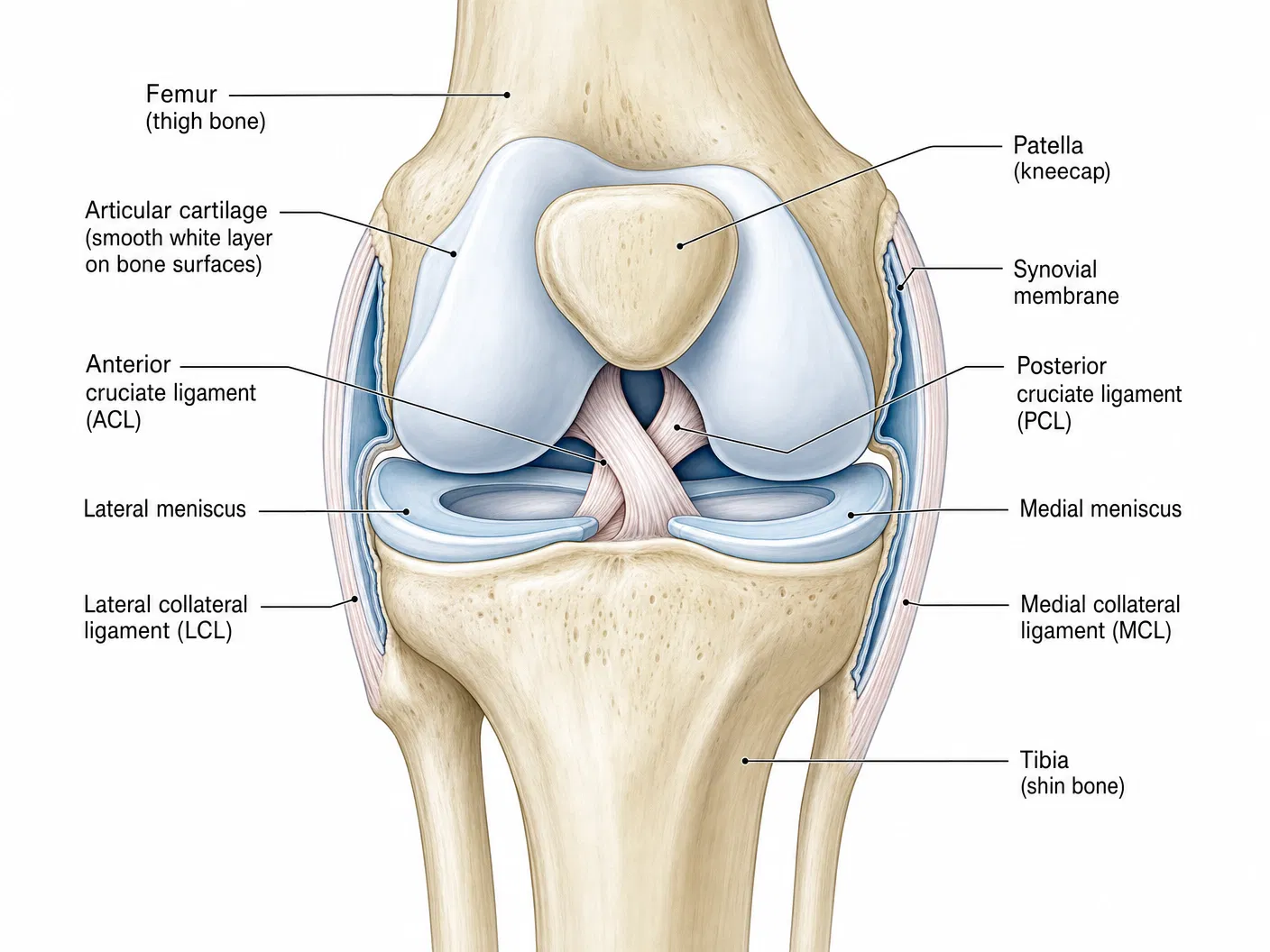
The knee is the largest joint in the body and one of the most complex. It is formed by three bones: the femur (thigh bone), the tibia (shin bone), and the patella (kneecap). The knee joint has three compartments — the medial (inner), lateral (outer), and patellofemoral (kneecap) compartment.
In a healthy knee, the bone surfaces within each compartment are covered with smooth articular cartilage (approximately 3–4 mm thick) that allows the joint to glide with minimal friction. The knee is stabilised by four main ligaments and is surrounded by a joint capsule lined with synovial membrane. Two crescent-shaped menisci sit between the femur and tibia, acting as shock absorbers and helping to distribute load evenly across the joint.
Why You May Need a Knee Replacement
Total knee replacement is considered when the articular cartilage has worn away significantly, causing bone to rub against bone. This results in pain, stiffness, swelling, and difficulty with everyday activities such as walking, climbing stairs, and getting in and out of chairs.
| Condition | Description |
|---|---|
| Osteoarthritis | The most common cause — gradual "wear and tear" degeneration of the cartilage, typically affecting patients over 55 years of age |
| Rheumatoid Arthritis | An autoimmune condition causing inflammation and destruction of the joint lining and cartilage |
| Post-Traumatic Arthritis | Arthritis developing after a significant knee injury (fracture, ligament injury, or meniscal damage) |
| Avascular Necrosis | Loss of blood supply to a section of bone, causing collapse of the joint surface |
Knee replacement is generally recommended when non-operative treatments — including physiotherapy, weight management, anti-inflammatory medications, and injections — have failed to provide adequate relief, and your quality of life is significantly affected.
The Decision to Operate
The decision to proceed with knee replacement is made together between you and Mr Dehne. There is no single test that determines when surgery is "needed" — it is based on your symptoms, functional limitations, examination findings, and imaging results.
Good Candidate If:
- • Significant daily pain limiting activities
- • Pain disturbs your sleep
- • Failed non-operative treatment for 3–6 months
- • X-rays show moderate to severe arthritis
- • Knee becoming increasingly stiff or deformed
- • Otherwise fit enough for surgery
Important Considerations
- • Elective procedure — timing is your choice
- • Designed to relieve pain, not create a "normal" knee
- • Most achieve 0–120° of flexion after surgery
- • Implant expected to last 20–25 years
- • Realistic expectations essential for satisfaction
Your New Knee — Implant Components
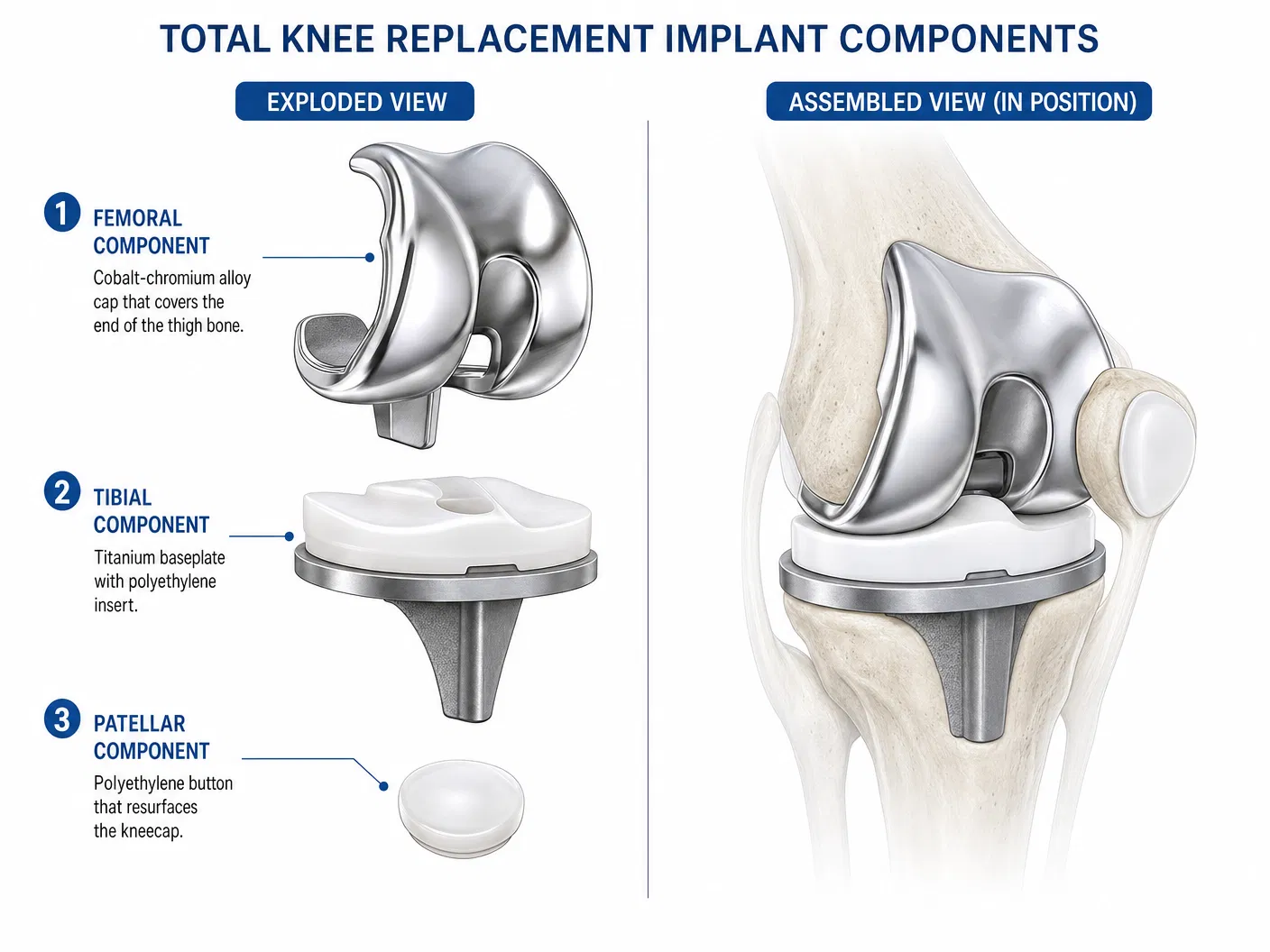
A total knee replacement resurfaces the worn joint surfaces with precision-engineered artificial components. The implant has three main parts:
| Component | Material | Function |
|---|---|---|
| Femoral Component | Cobalt-chromium alloy | Covers the end of the thigh bone; shaped to replicate the natural curve of the femur |
| Tibial Component | Titanium baseplate + polyethylene insert | Covers the top of the shin bone; the plastic insert provides a smooth gliding surface |
| Patellar Component | Polyethylene button | Resurfaces the underside of the kneecap (used in some patients) |
The components are typically fixed to the bone using polymethylmethacrylate (PMMA) bone cement, which sets within minutes and provides immediate stability. Modern knee implants are designed to replicate the natural kinematics of the knee, and survival rates exceed 95% at 15 years based on national joint registry data.
The Surgical Procedure
Total knee replacement is performed under anaesthesia — typically a spinal anaesthetic (which numbs you from the waist down) combined with sedation. General anaesthesia is also available if preferred. The operation takes approximately 60–90 minutes.
Approach
A midline incision (approximately 15–20 cm) is made over the front of the knee. The joint is accessed through a medial parapatellar approach.
Bone Preparation
Precision cutting guides (jigs) are used to remove the worn cartilage and a thin layer of bone from the femur, tibia, and patella at precise angles.
Trial Components
Temporary implants are inserted to check fit, alignment, stability, and range of motion. Adjustments are made until the knee is well-balanced.
Final Implantation
The definitive implants are cemented into place. The polyethylene insert is locked into the tibial baseplate.
Closure
The joint capsule and skin are closed in layers. A local anaesthetic cocktail is injected around the knee for pain relief.
Dressing
A sterile dressing and compression bandage are applied. No drain is typically required.
The JointClinics Fast Recovery Programme
Our Fast Recovery Programme represents the gold standard in perioperative care for joint replacement surgery. This evidence-based Enhanced Recovery After Surgery (ERAS) approach has been shown to reduce hospital stay, decrease complications, improve pain control, and accelerate return to normal function.
Minimise Surgical Stress
Spinal anaesthesia, tranexamic acid, local infiltration, meticulous soft-tissue handling
Multimodal Pain Control
Paracetamol, anti-inflammatories, nerve blocks, local infiltration — minimising opioids
Early Mobilisation
Standing and walking on the day of surgery (Day 0) with physiotherapy support
Optimised Nutrition
No prolonged fasting; clear fluids up to 2 hours before; early eating after surgery
Complication Prevention
DVT prophylaxis, infection prevention bundle, blood conservation strategies
Patient Empowerment
Comprehensive education, clear expectations, active participation in recovery
What the Evidence Shows
Reduced hospital stay: from 5–7 days to 1–2 days
Fewer complications: reduced transfusion, infection, and DVT rates
Better pain control with fewer opioid side effects
Faster functional recovery milestones
No increase in 30-day readmission rates
Higher patient satisfaction scores
Preparing for Surgery (Prehabilitation)
Preparation before surgery — "prehabilitation" — is a critical component of the Fast Recovery Programme. Research shows that patients who are physically and mentally prepared before surgery recover faster and have better outcomes.
4–6 Weeks Before Surgery
Physical Preparation
- • Daily quadriceps strengthening exercises
- • Walk 20–30 minutes daily
- • Practice using crutches or walking frame
- • Achieve best possible range of motion
Medical Optimisation
- • Stop smoking at least 4 weeks before
- • Reduce alcohol intake
- • Optimise diabetes control (HbA1c < 69)
- • Treat anaemia if haemoglobin is low
Practical Preparation
- • Arrange transport home from hospital
- • Prepare your home: remove trip hazards, consider raised toilet seat and shower stool
- • Stock freezer with easy-to-prepare meals
- • Arrange help for the first 1–2 weeks
- • No food 6 hours before surgery; clear fluids up to 2 hours before
What to Expect on the Day of Surgery
You will arrive at the hospital on the morning of your surgery. The nursing team will confirm your details, mark your surgical site, and prepare you for theatre. You will meet your anaesthetist to discuss your anaesthetic plan.
The operation typically takes 60–90 minutes. After surgery, you will spend approximately 1 hour in the recovery room while the nursing team monitors your observations and ensures your pain is well controlled.
Day 0 Goals (Afternoon/Evening of Surgery)
As part of the Fast Recovery Programme, our physiotherapy team will visit you on the day of surgery:
Your Hospital Stay
Under the Fast Recovery Programme, most patients stay in hospital for 1–2 nights. Some patients who meet specific criteria may be suitable for same-day discharge.
Discharge Criteria
Walk independently with crutches or frame (approximately 30 metres)
Climb stairs safely (if needed at home)
Get in and out of bed independently
Bend your knee to at least 70–80°
Manage pain with oral medications
Pass urine normally
No signs of complications
Pain Management
Good pain control is essential for early mobilisation and recovery. The Fast Recovery Programme uses a "multimodal" approach — combining several different types of pain relief for maximum effect with minimum side effects.
| Method | Timing | Details |
|---|---|---|
| Local Anaesthetic Infiltration | During surgery | Cocktail injected around the knee at end of operation |
| Paracetamol | Regular (4× daily) | Safe, effective baseline — take regularly, not just when in pain |
| Anti-inflammatory | Regular (2–3× daily) | Reduces inflammation and pain; take with food |
| Gabapentin/Pregabalin | As prescribed | Reduces nerve-related pain and improves sleep |
| Opioids | As needed | Breakthrough pain only; aim to stop within 2–4 weeks |
| Ice Therapy | 20 min, 3–4× daily | Reduces swelling and provides natural pain relief |
Key Principles
- • Take regular painkillers on schedule for the first 2 weeks
- • Pain typically peaks at days 2–3, then gradually improves
- • Swelling is normal and may persist for 3–6 months
- • Aim to reduce and stop opioid painkillers within 2–4 weeks
Rehabilitation Programme
Rehabilitation is the most important factor in determining your outcome after knee replacement. The programme is progressive, building on each stage as your knee heals and strengthens.
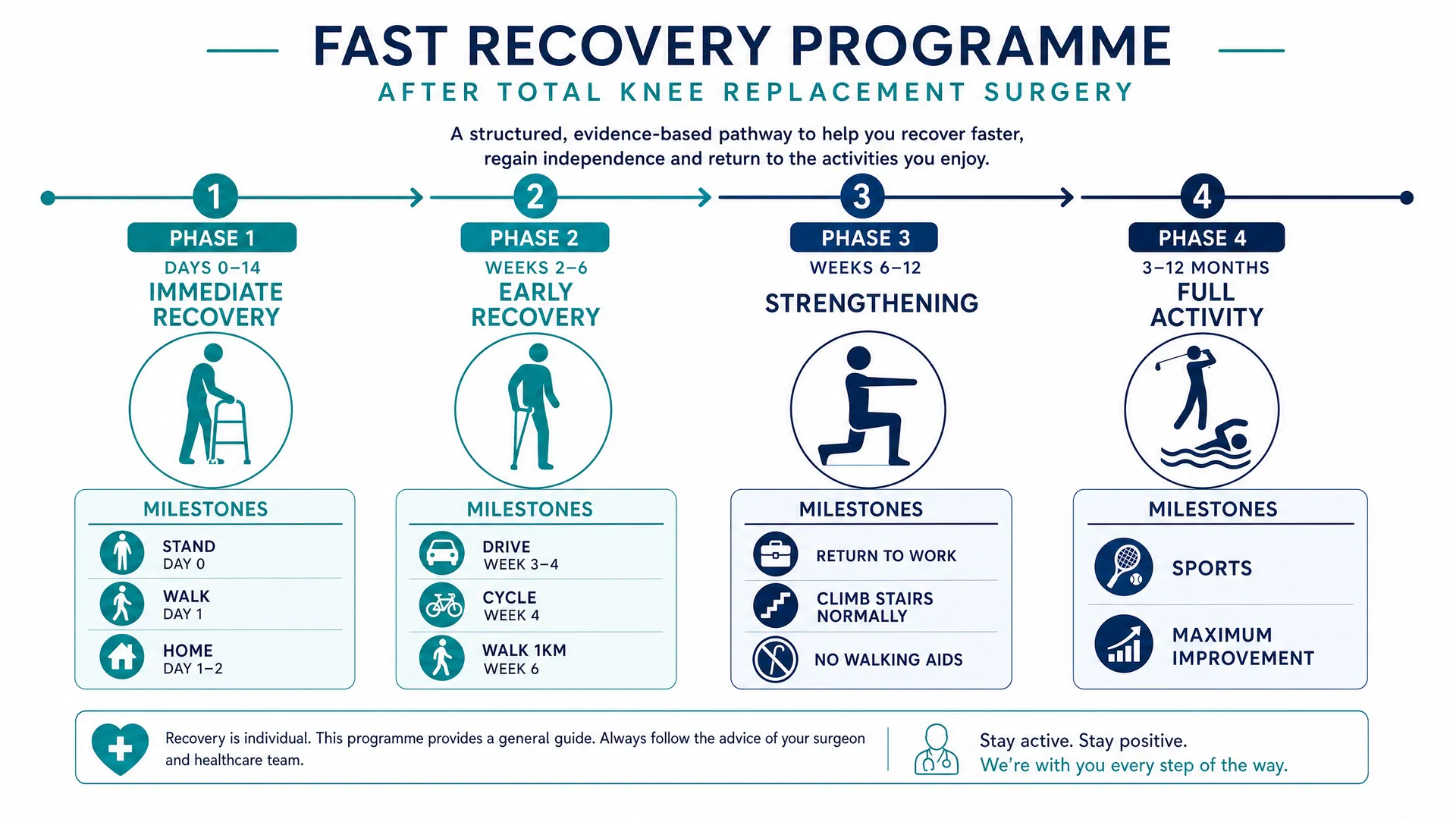
Phase 1: Immediate Post-Operative (Days 0–14)
Goals: Control pain and swelling, protect the wound, achieve early mobility milestones
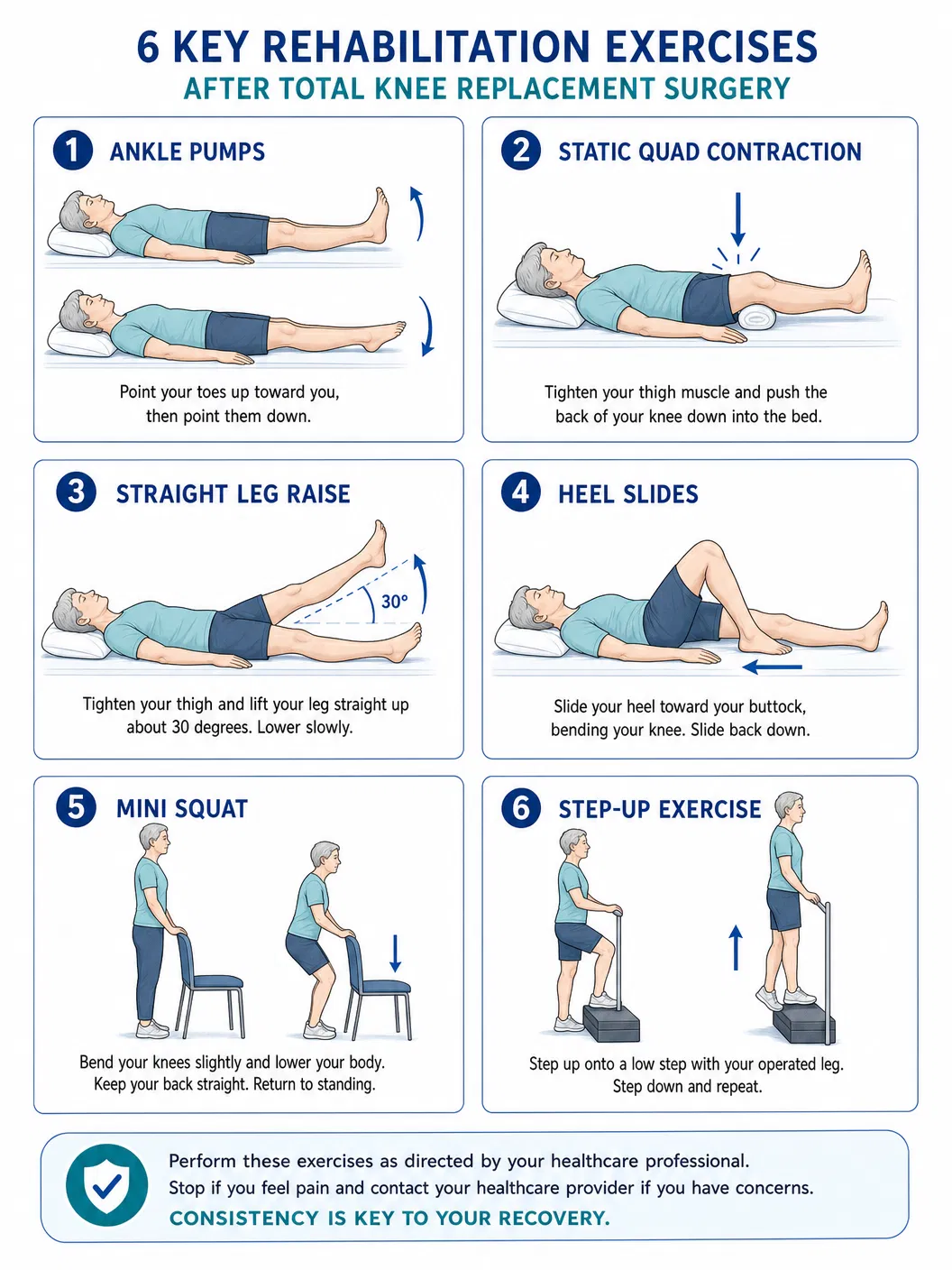
| Exercise | Sets/Reps | Frequency |
|---|---|---|
| Ankle pumps | 20 reps | Every hour |
| Static quad contractions | 10 × 5-sec holds | 4× daily |
| Straight leg raises | 3 × 10 reps | 3× daily |
| Heel slides | 3 × 10 reps | 4× daily |
| Knee extension stretch | 5 minutes | 4× daily |
Day 0: Stand and take first steps with frame
Day 1: Walk 30+ metres; climb stairs
Day 7: Walk 100+ metres; knee bending to 70–80°
Day 14: Walk short distances without crutches; knee bending to 90°
Phase 2: Early Recovery (Weeks 2–6)
Goals: Restore range of motion (target 0–110°), build muscle strength, increase walking distance
- • Heel slides (progressing range), mini squats, step-ups
- • Stationary cycling (high seat): 10–20 minutes daily
- • Straight leg raises in all directions
- • Knee extension with resistance band
Week 3: Walk outdoors with one crutch; drive short distances (automatic, left knee)
Week 4: Walk 500+ metres; begin stationary cycling
Week 6: Walk 1 km+; knee bending to 100–110°; wean off crutches
Phase 3: Strengthening (Weeks 6–12)
Goals: Restore full strength, improve balance and proprioception, return to most daily activities
- • Squats and lunges (progressing depth)
- • Leg press and step-ups (increasing height)
- • Balance exercises (single leg stand)
- • Swimming/aqua exercises: 20–30 min, 2–3× per week
- • Outdoor cycling: 20–30 min, 3–4× per week
Week 8: Walk 2+ km without aids; return to light work
Week 10: Climb stairs normally (step over step)
Week 12: Knee bending to 115–120°; return to driving (right knee)
Phase 4: Return to Full Activity (3–12 Months)
Goals: Maximise strength and endurance, return to recreational activities
- • Continue strengthening 2–3× per week indefinitely
- • Gradually return to sports (golf, swimming, cycling, walking, doubles tennis)
- • Maximum improvement typically achieved by 12 months
- • Some patients continue to improve up to 2 years after surgery
Returning to Activities
The following timelines are general guides. Your individual recovery may be faster or slower depending on your fitness, the complexity of your surgery, and your progress with rehabilitation.
| Activity | Timeline | Notes |
|---|---|---|
| Driving (automatic, left knee) | 3–4 weeks | When safe to emergency stop |
| Driving (right knee/manual) | 6–8 weeks | Must brake firmly without pain |
| Return to desk work | 4–6 weeks | Elevate leg; take regular breaks |
| Return to manual work | 8–12 weeks | Depends on physical demands |
| Swimming | 6 weeks | Once wound fully healed |
| Stationary cycling | 4–6 weeks | Start with high seat position |
| Outdoor cycling | 8–12 weeks | Flat terrain initially |
| Golf | 12 weeks | Start with putting/chipping |
| Walking holidays | 3–6 months | Build distance gradually |
| Kneeling | Variable | May be uncomfortable; use cushion |
| Running/high-impact | Not recommended | Increases implant wear |
Risks and Complications
Total knee replacement is a safe and well-established procedure, but like all surgery, it carries risks. Mr Dehne will discuss these with you in detail before you consent to surgery.
Common (more than 1 in 20 patients)
- Pain and swelling: Expected after surgery; gradually improves over weeks to months
- Stiffness: Some limitation of movement is normal; physiotherapy is essential
- Bruising: May extend down the leg; resolves over 2–4 weeks
- Numbness: A patch on the outer side of the knee is common and usually permanent but not troublesome
Uncommon (1 in 20 to 1 in 100 patients)
- Infection (1–2%): We use antibiotics, laminar flow theatres, and strict sterile technique. Further surgery may be needed if infection occurs.
- Blood clots — DVT/PE (1–2%): Blood-thinning medication and early mobilisation reduce this risk.
- Stiffness requiring manipulation (3–5%): If adequate movement is not achieved by 6–8 weeks, manipulation under anaesthesia may be recommended.
- Wound healing problems (5–7%): Prolonged drainage, skin edge necrosis, or delayed healing.
Rare (fewer than 1 in 100 patients)
- Nerve or blood vessel injury: Damage to the peroneal nerve or popliteal artery is rare but serious
- Fracture: A crack in the bone around the implant during or after surgery
- Implant loosening: Typically a long-term problem (10–20 years); may require revision surgery
- Instability: Feeling of the knee "giving way"; may require further surgery
Long-term: Modern implants last 20–25 years in the majority of patients. Younger, more active patients may wear out their implant sooner. You should inform your dentist and any doctor performing invasive procedures that you have a knee replacement.
Frequently Asked Questions
How long does the operation take?
The operation typically takes 60–90 minutes. You will be in the operating theatre for approximately 90–120 minutes in total including anaesthetic preparation.
How long will I stay in hospital?
Under the Fast Recovery Programme, most patients stay 1–2 nights. Some patients are suitable for same-day discharge depending on individual progress and home circumstances.
How long will it take to recover?
Most patients return to daily activities within 6–12 weeks. Maximum improvement is typically achieved by 12 months, although some patients continue to improve for up to 2 years.
Will my knee feel normal?
A replaced knee will not feel identical to a natural knee. Most patients describe it as feeling "different but much better." The vast majority report significant pain relief and improved function.
Can I kneel after knee replacement?
Many patients can kneel, although it may feel uncomfortable. Using a cushion helps. Kneeling will not damage the implant.
How long will the implant last?
Over 95% of modern knee implants are still functioning well at 15 years, and approximately 85% at 25 years, based on national joint registry data.
Can I have an MRI after knee replacement?
Yes. Modern knee implants are MRI-compatible. Inform the radiographer about your implant before any MRI scan.
When can I fly after surgery?
Short-haul flights (under 4 hours) are generally safe from 6 weeks. For long-haul flights, wait at least 12 weeks and wear compression stockings.
Do I need antibiotics before dental treatment?
Current UK guidelines do not routinely recommend antibiotic prophylaxis before dental procedures for patients with joint replacements. However, inform your dentist about your implant.
Warning Signs — When to Seek Help
Contact JointClinics, your GP, or attend A&E if you experience:
Possible Infection
Increasing redness, warmth, or swelling around wound
Wound discharge (cloudy, green, or foul-smelling)
Fever (temperature above 38°C)
Feeling generally unwell, shivery, or flu-like
Possible Blood Clot (DVT/PE)
Sudden calf pain, swelling, or tenderness
Sudden shortness of breath or chest pain
Coughing up blood
If you experience chest pain, sudden breathlessness, or coughing up blood — call 999 immediately.
References
- Kehlet H. Multimodal approach to control postoperative pathophysiology and rehabilitation. Br J Anaesth. 1997;78(5):606-617.
- Riga M, et al. Enhanced recovery after surgery (ERAS) protocols for total joint replacement surgery. SICOT J. 2023;9:E1.
- Castorina S, et al. Clinical evidence of traditional vs fast track recovery methodologies after total arthroplasty. Muscles Ligaments Tendons J. 2018;7(3):504-513.
- Husted H, et al. Fast-track hip and knee arthroplasty: clinical and organizational aspects. Acta Orthop. 2012;83(sup1):39-43.
- Picart B, et al. Implementation and results of an enhanced recovery program for knee replacement surgery. Orthop Traumatol Surg Res. 2021;107(3):102832.
- Arienti C, et al. Fast-track rehabilitation after TKA reduces length of stay. Int J Environ Res Public Health. 2020;17(23):9061.
- National Joint Registry for England, Wales, Northern Ireland and the Isle of Man. 20th Annual Report. 2023.
- Ishaku Z, et al. ERAS Pathways in Elective Total Joint Arthroplasty. Cureus. 2025;17(9):e382306.
- He P, et al. Assessment of ERAS protocol in elderly patients undergoing primary TKA. Medicine. 2026;105(12):e41892.
- Joshi GP, et al. ERAS Society recommendations for perioperative care in TJR. Acta Orthop. 2020;91(1):3-19.