ACL Reconstruction
Quadrupled semitendinosus graft with internal brace augmentation — a modern, evidence-based approach to restoring knee stability
Understanding Your Knee — Anatomy
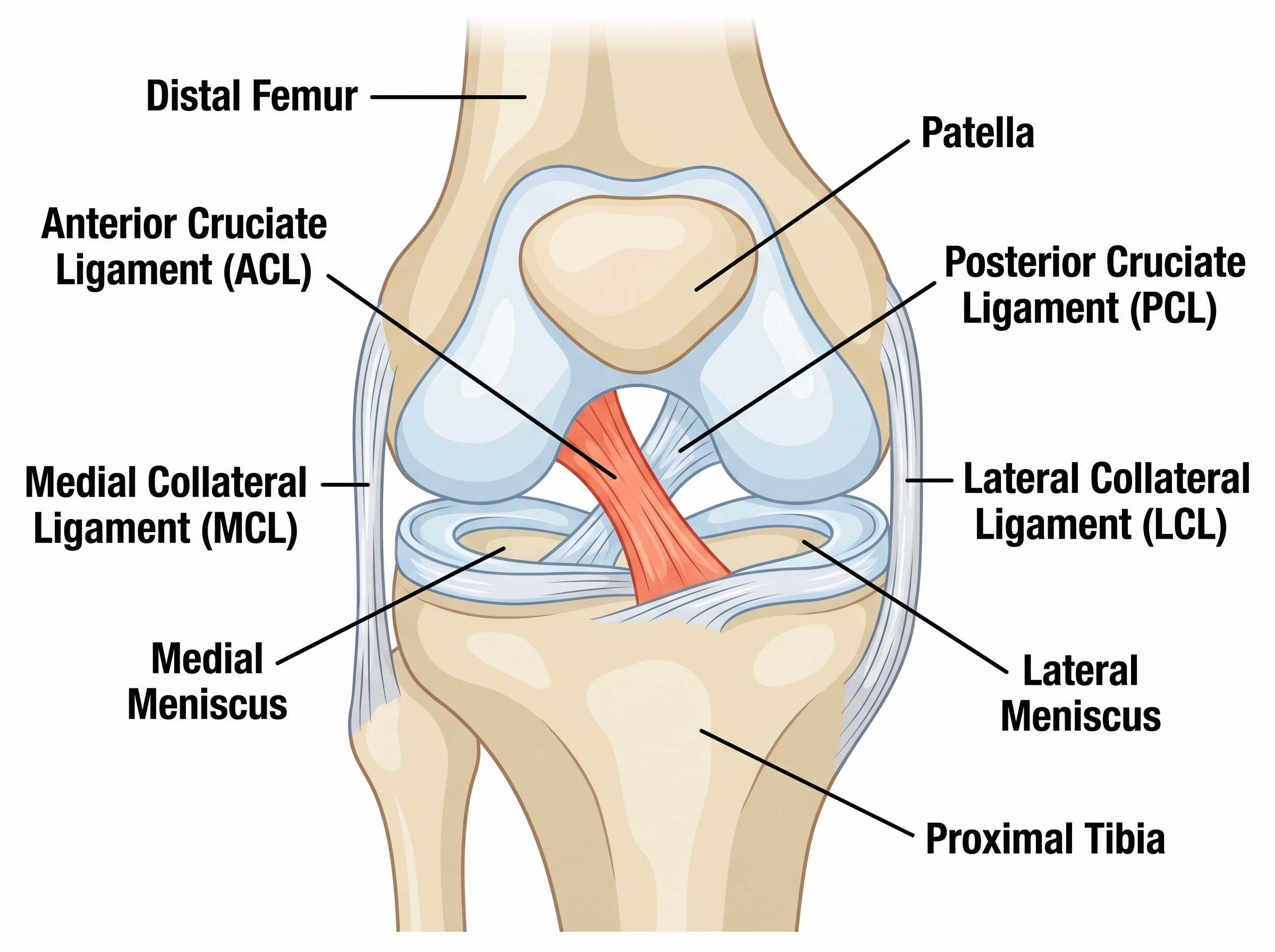
The knee is the largest and most complex joint in the body. It is formed by three bones: the femur (thigh bone), the tibia (shin bone), and the patella (kneecap). Four major ligaments provide stability to the knee, working together to control movement and prevent abnormal motion.
Anterior Cruciate Ligament (ACL) — prevents the tibia from sliding forward and controls rotational stability
Posterior Cruciate Ligament (PCL) — prevents the tibia from sliding backward
Medial Collateral Ligament (MCL) — stabilises the inner side of the knee
Lateral Collateral Ligament (LCL) — stabilises the outer side of the knee
What is the ACL and What Does It Do?
The ACL is a strong band of tissue that runs diagonally through the centre of the knee, connecting the femur to the tibia. It is the primary restraint against forward translation of the tibia and is critical for rotational stability of the knee.
The ACL is essential for activities that involve pivoting, cutting, or sudden changes of direction. Without a functioning ACL, the knee may feel unstable during these movements, leading to episodes of "giving way" that can damage the meniscus and articular cartilage over time.
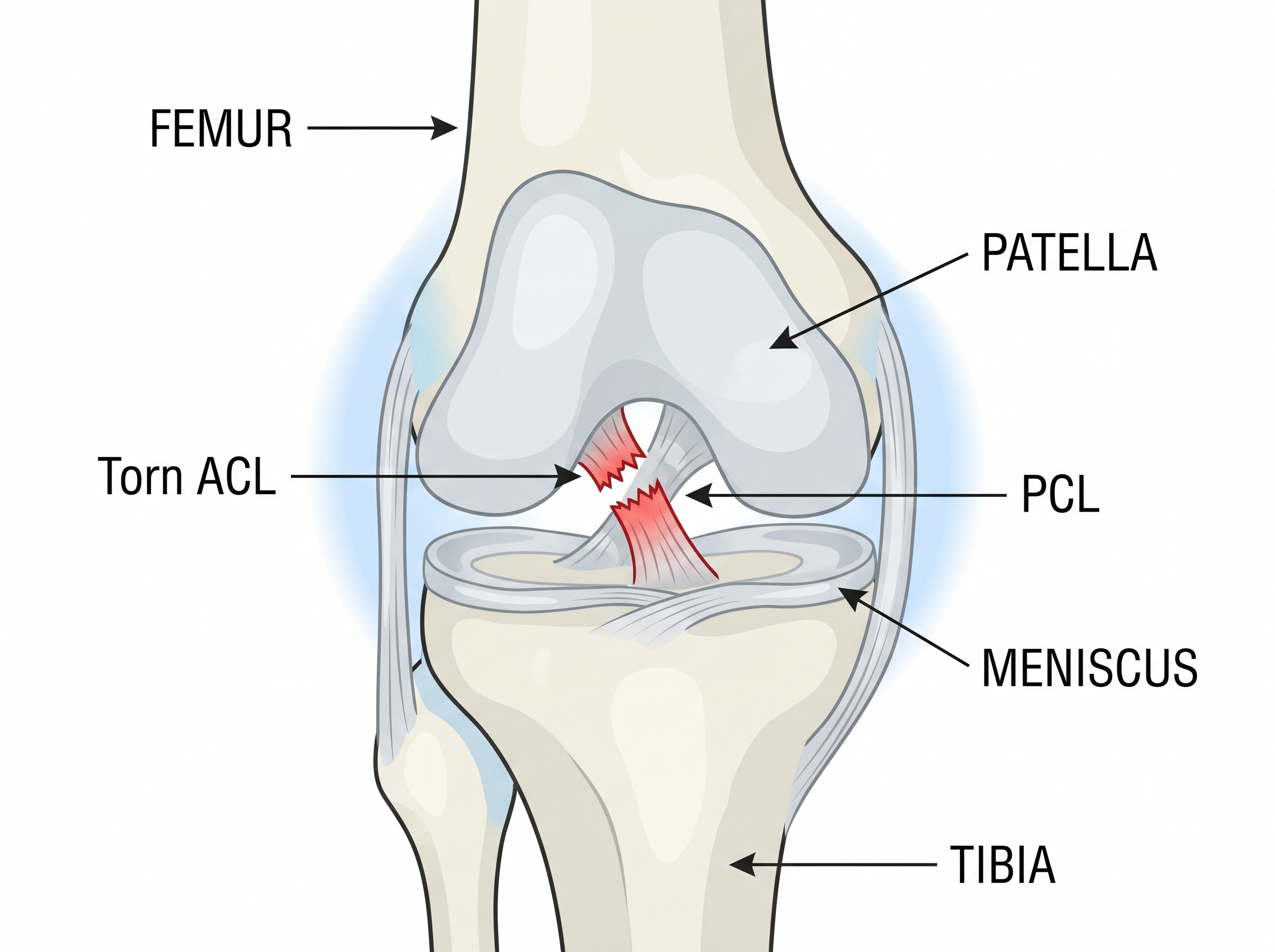
How Does the ACL Get Injured?
ACL injuries are common in sports that involve sudden stops, changes of direction, or landing from jumps. Approximately 70% of ACL injuries occur through non-contact mechanisms.
| Mechanism | Description | Common Sports |
|---|---|---|
| Pivot/twist | Sudden change of direction with foot planted | Football, basketball, netball |
| Landing | Landing from a jump with knee extended or valgus | Gymnastics, volleyball, skiing |
| Deceleration | Sudden stopping with knee near full extension | Football, rugby, tennis |
| Direct contact | Blow to the outer side of the knee | Rugby, football, martial arts |
At the time of injury, patients often report hearing or feeling a "pop," followed by rapid swelling (within 2–4 hours) and difficulty bearing weight. The knee may feel unstable or "loose."
Do I Need Surgery?
Not everyone with an ACL tear requires surgery. The decision depends on your activity level, symptoms, associated injuries, and goals. Mr Dehne will discuss the options with you in detail.
| Surgery Recommended | Non-Operative May Be Suitable |
|---|---|
| Young, active patients wanting to return to pivoting sports | Older patients with low activity demands |
| Recurrent episodes of instability (giving way) | No episodes of instability with daily activities |
| Associated meniscal tear requiring repair | Isolated ACL tear with good muscle control |
| Occupational requirements (physical jobs, military, police) | Willing to modify activities and avoid pivoting sports |
The Surgical Technique
Quadrupled Semitendinosus Graft with Internal Brace Augmentation
Mr Dehne uses a modern technique combining a quadrupled semitendinosus hamstring graft with an internal brace (suture tape augmentation). This approach maximises graft protection during healing while minimising donor-site morbidity.
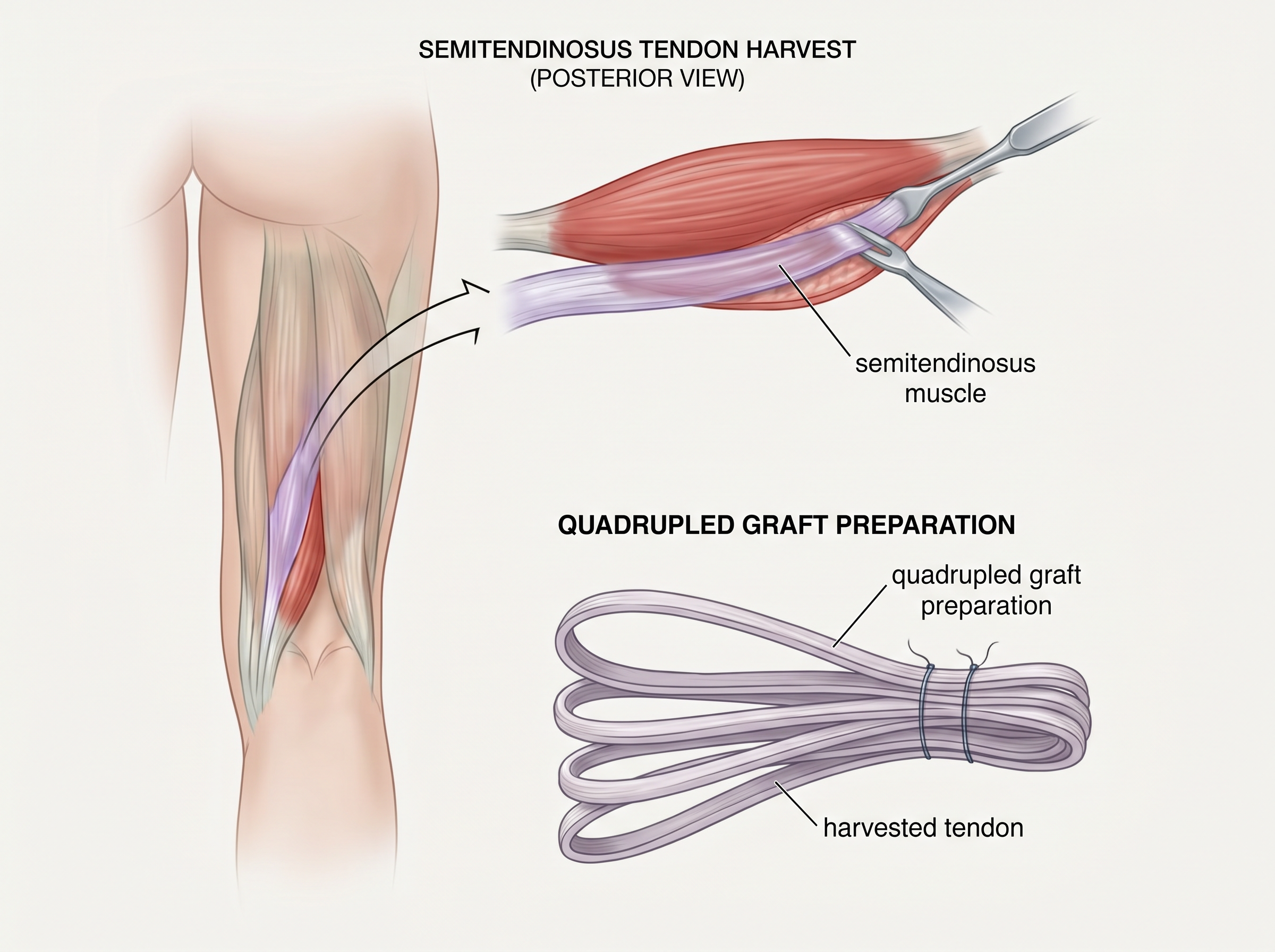
The Graft: Quadrupled Semitendinosus
The semitendinosus tendon is one of the hamstring tendons on the inner side of the knee. It is harvested through a small incision and folded four times (quadrupled) to create a thick, robust graft bundle that closely matches the diameter and strength of the native ACL. Key advantages include reduced donor-site morbidity, preservation of hamstring strength for deep knee flexion, and faster return of hamstring function compared to techniques that harvest both tendons.
The Internal Brace: Suture Tape Augmentation
The internal brace is a high-strength suture tape (typically 2.0mm FiberTape) placed alongside the graft within the bone tunnels. It acts as a "seatbelt" for the new ligament — sharing the load with the graft and protecting it from excessive elongation during the early healing phase when the graft is at its weakest (the period of "ligamentisation").
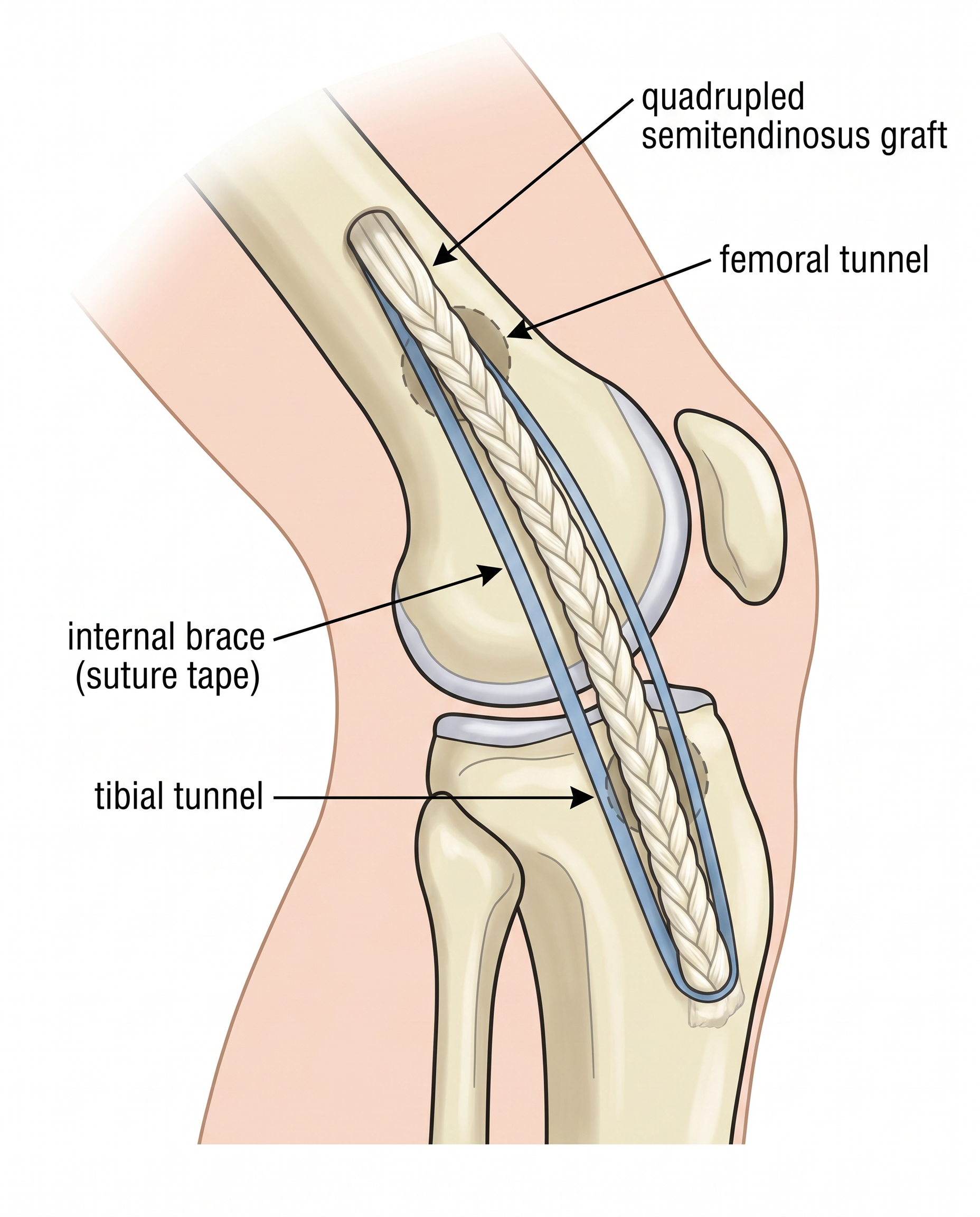
How the Surgery is Performed
The entire procedure typically takes 60–90 minutes. It is performed arthroscopically (keyhole surgery) as a day-case procedure, meaning you will usually go home on the same day. The graft is fixed in anatomical bone tunnels using cortical suspensory fixation buttons, and the internal brace is independently tensioned to protect the graft from day one.
Evidence Supporting This Technique
| Study | Key Finding |
|---|---|
| Wallace et al. (2024) | Suture tape augmentation of four-strand semitendinosus graft significantly improves time-zero biomechanical properties. 2.0mm tape superior to 1.3mm with increased load to failure and construct stiffness. |
| Bachmaier et al. (2018) | Suture tape reinforcement reduces graft elongation by 15–56% and increases overall construct stiffness — critical during the first 6–12 weeks of graft remodelling. |
| Wilson et al. (2023) | 5-year follow-up: remarkably low failure rate of only 1.1% — significantly lower than the 5–15% revision rates for standard ACL reconstruction without augmentation. |
| Maginnis et al. (2024) | Systematic review (AJSM): all graft types with suture tape augmentation showed no disadvantage vs standard reconstruction, with reduced laxity (0.8mm vs 1.9mm, P<0.05). |
Summary: The technique of using only the semitendinosus tendon (preserving the gracilis) combined with internal brace augmentation represents an evolution in ACL surgery that maximises graft protection while minimising donor-site morbidity. The internal brace acts as a secondary stabiliser during the vulnerable period of graft remodelling, after which the biological graft assumes the primary load-bearing role.
Preparing for Your Surgery
Optimal preparation before surgery ("prehabilitation") has been shown to improve outcomes after ACL reconstruction. The Melbourne ACL Rehabilitation Protocol recommends achieving specific pre-operative benchmarks before proceeding to surgery.
Pre-operative Checklist
Complete your prehabilitation exercises as prescribed by your physiotherapist
Attend your pre-operative assessment appointment
Stop anti-inflammatory medications (e.g., ibuprofen) 7 days before surgery
Stop aspirin 5 days before surgery (unless otherwise advised)
Do not eat or drink for 6 hours before your scheduled surgery time
Arrange transport home — you will not be able to drive after surgery
Prepare your home: place items at waist height, clear trip hazards
Obtain crutches (these will be provided if not already available)
Wear loose, comfortable clothing on the day of surgery
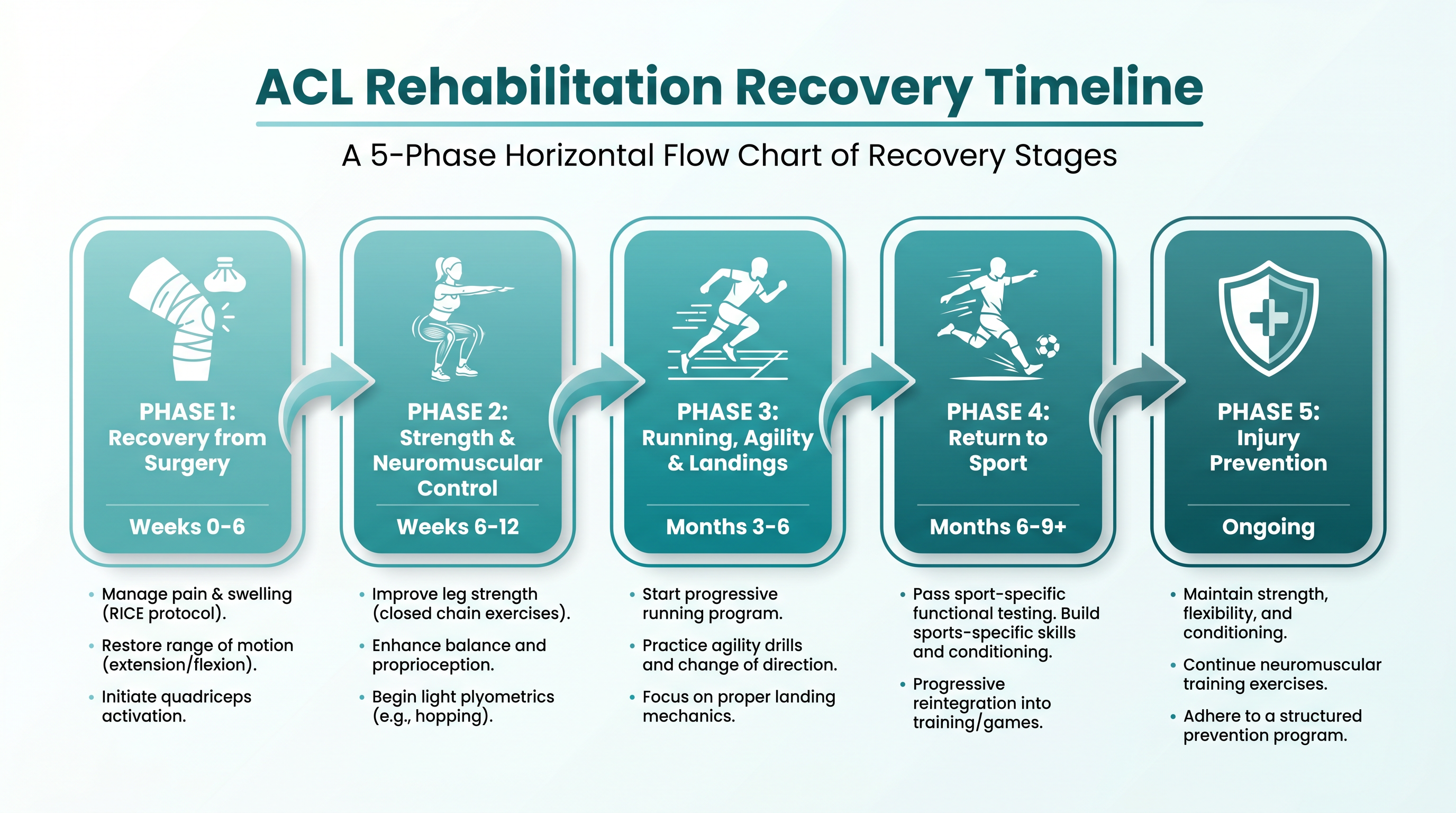
Rehabilitation — The Melbourne ACL Protocol
Rehabilitation is criterion-based, not time-based. You progress through each phase by achieving specific functional milestones, not simply by waiting a set number of weeks. This ensures your knee is truly ready for the next level of loading.
Phase 1: Recovery from Surgery
Weeks 0–2
Goals: Restore full knee extension (0°), reduce swelling, achieve good quadriceps activation, independent straight-leg raise without lag
Progression criteria: Full extension, minimal swelling, good quad control
Phase 2: Strength & Neuromuscular Control
Weeks 2–12
Goals: Full range of motion, single-leg balance, leg press at 1.5× body weight, pain-free walking without limp
Progression criteria: Limb symmetry index >70% for strength
Phase 3: Running, Agility & Landings
Months 3–6
Goals: Return to straight-line running, introduce change-of-direction drills, hop testing, sport-specific movements
Progression criteria: Hop test symmetry >90%, no pain or swelling with running
Phase 4: Return to Sport
Months 6–12
Goals: Full sport-specific training, match fitness, psychological readiness, pass Melbourne Return to Sport Score (MRSS 2.0)
Progression criteria: All functional tests >90% symmetry, MRSS score satisfactory
Phase 5: Injury Prevention
Ongoing
Goals: Maintenance programme to reduce re-injury risk, neuromuscular training, landing mechanics, ongoing strength work
Progression criteria: Lifelong commitment to prevention exercises
Risks and Complications
ACL reconstruction is a well-established and safe procedure. However, like all surgery, it carries some risks. Mr Dehne will discuss these with you in detail before your operation.
| Complication | Frequency | Management |
|---|---|---|
| Infection | < 1% | Antibiotics; rarely requires washout |
| Blood clot (DVT/PE) | < 1% | Blood thinners, compression stockings, early mobilisation |
| Stiffness (arthrofibrosis) | 2–5% | Aggressive physiotherapy; rarely manipulation under anaesthesia |
| Graft failure/re-rupture | 1.1% at 5 years (with internal brace) | Revision ACL reconstruction |
| Numbness around incision | 10–20% | Usually resolves over 6–12 months |
| Donor-site pain | 5–10% | Usually settles within 3–6 months |
Frequently Asked Questions
How long until I can return to sport?
Return to sport is criterion-based, not time-based. Most patients achieve full return between 9–12 months, but this depends on passing all functional tests with >90% limb symmetry. Rushing back increases re-injury risk.
Will I need to stay in hospital?
No — ACL reconstruction is performed as a day-case procedure. You will go home on the same day with crutches, pain medication, and a detailed rehabilitation plan.
How strong will my new ACL be?
The quadrupled semitendinosus graft with internal brace has been shown to exceed the strength of the native ACL at time zero. Over time, the graft undergoes biological remodelling (ligamentisation) and matures into a functional ligament. The internal brace protects it during this vulnerable period.
What is the success rate?
With the internal brace technique, published data shows a revision rate of only 1.1% at 5-year follow-up. Over 90% of patients report good to excellent outcomes and return to their desired activity level.
Can I fly after surgery?
Short-haul flights (under 4 hours) are generally safe after 2 weeks, provided you perform regular ankle exercises and stay hydrated. For long-haul flights, wait at least 4–6 weeks and consider compression stockings.
When can I drive?
For left knee surgery with an automatic car, you may be able to drive at 2 weeks. For right knee surgery, driving typically resumes at 4–6 weeks once you can safely perform an emergency stop.
Warning Signs — When to Contact Us
After surgery, contact Mr Dehne's team or attend A&E immediately if you experience:
Increasing pain not controlled by your prescribed medication
Calf pain, swelling, or tenderness (possible DVT)
Chest pain or sudden shortness of breath (possible pulmonary embolism)
Fever above 38°C or increasing redness/discharge from the wound
Numbness or tingling in the foot that does not resolve
Inability to straighten the knee (may indicate locked knee from meniscal tissue)
References
- Wallace GJ, et al. Suture Augmentation of a Four-Strand Semitendinosus Graft Improves Time-Zero Biomechanical Properties. Arthroscopy. 2024;40(1):e1-e10.
- Wilson WT, et al. Outcomes of ACL Reconstruction with Independently Tensioned Suture Tape Augmentation at 5-Year Follow-Up. Am J Sports Med. 2023;51(14):3623-3631.
- Maginnis C, et al. Analysis of Graft Types Augmented With an Internal Brace for ACL Reconstruction: A Systematic Review. Am J Sports Med. 2024;52(9):2415-2423.
- Bachmaier S, et al. Independent Suture Tape Reinforcement of Small and Standard Diameter Grafts for ACL Reconstruction: A Biomechanical Full Construct Model. Arthroscopy. 2018;34(2):490-499.
- Cooper R, Hughes M. Melbourne ACL Rehabilitation Guide 2.0. team-acl.com. 2022.
- Thilak J, Panicker J. Arthroscopic Remnant Preservation ACL Reconstruction Using Quadrupled Semitendinosus Autograft with Internal Brace. J ISAKOS. 2025.