Hip Replacement Surgery
Piriformis-sparing posterior approach — enhanced stability, faster recovery, and excellent long-term outcomes
Understanding Your Hip Joint
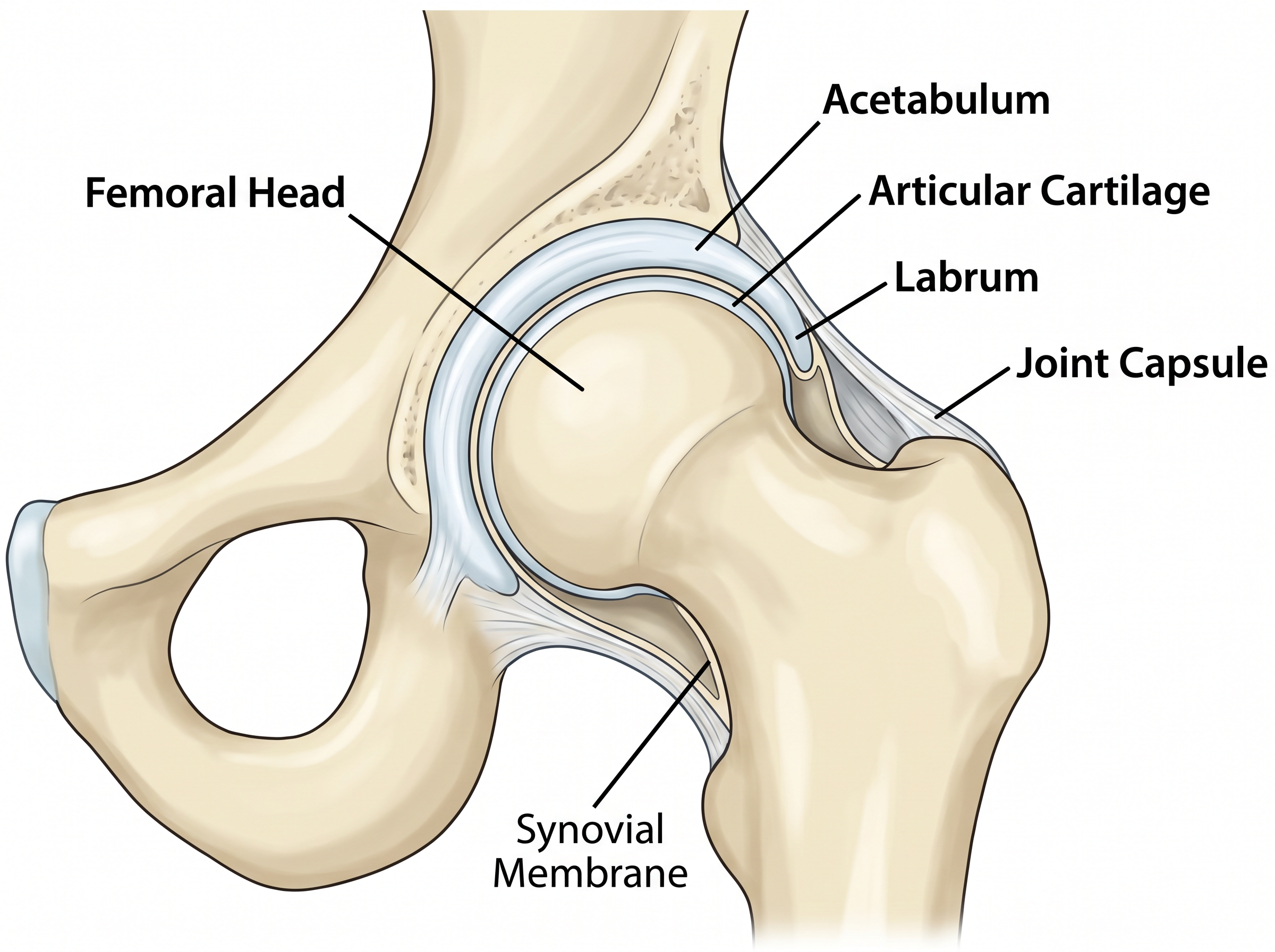
The hip is a ball-and-socket joint formed by the femoral head (ball) sitting within the acetabulum (socket) of the pelvis. It is one of the largest and most stable joints in the body, designed to bear the weight of the upper body while allowing a wide range of movement.
The joint is surrounded by a strong capsule and stabilised by powerful muscles. The short external rotator muscles on the back of the hip are particularly important for stability and are central to Mr Dehne's surgical technique.
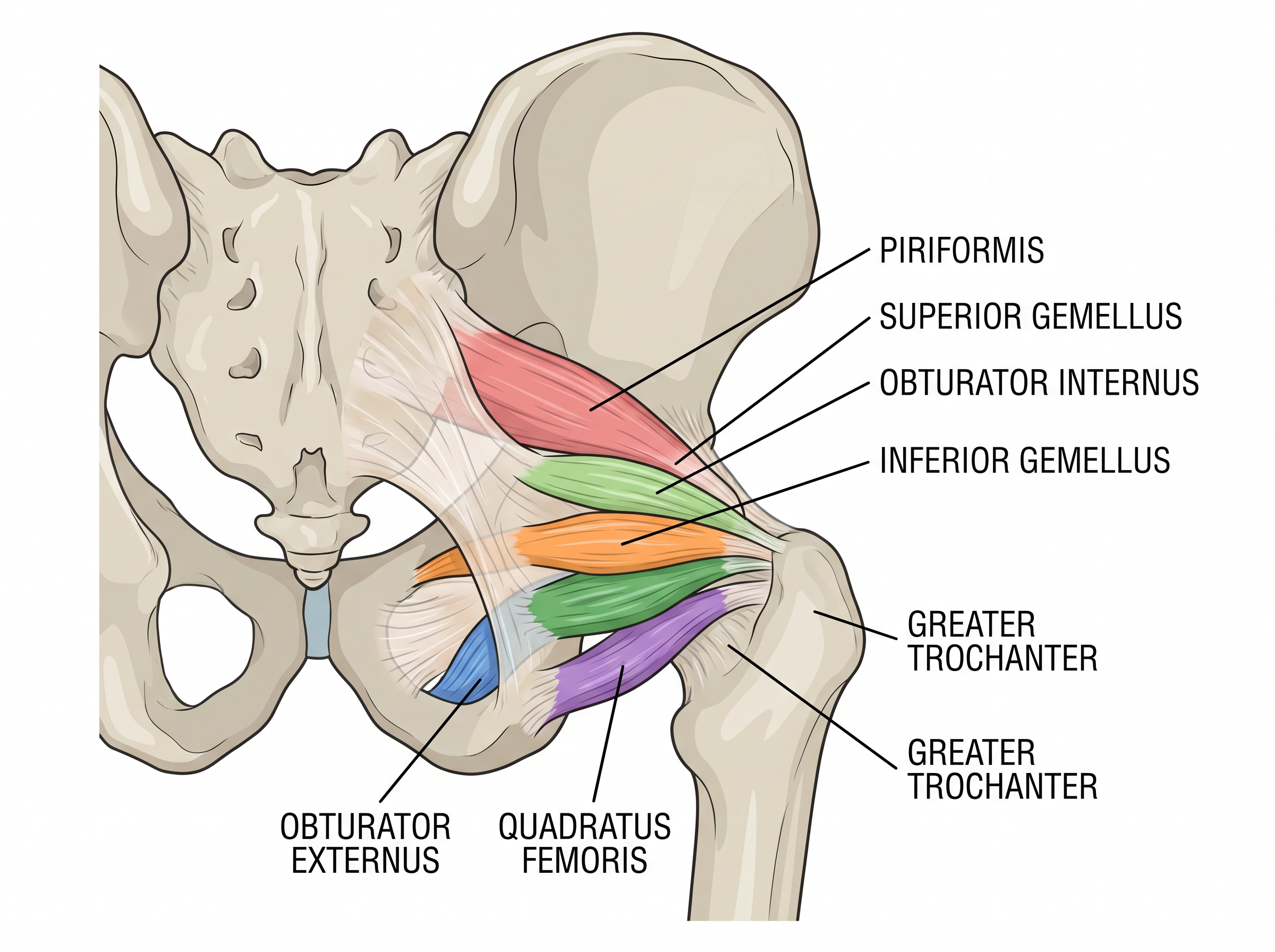
The Short External Rotator Muscles
The short external rotators are a group of muscles on the back of the hip that provide dynamic stability. The most important of these is the piriformis muscle, which acts as the primary dynamic stabiliser of the hip joint posteriorly. In traditional posterior approach hip replacement, the piriformis is cut and may not heal reliably — this is a key factor in post-operative dislocation risk.
When Hip Replacement Is Needed
| Condition | Description |
|---|---|
| Osteoarthritis | The most common reason — wear-and-tear degeneration of the joint cartilage causing bone-on-bone contact |
| Rheumatoid arthritis | Autoimmune inflammation destroying the joint surfaces |
| Avascular necrosis | Loss of blood supply to the femoral head causing bone collapse |
| Hip fracture | Displaced fractures of the femoral neck in older patients |
| Dysplasia | Abnormal hip development causing premature arthritis |
Signs That Surgery May Be Appropriate
Pain that significantly limits your daily activities (walking, stairs, dressing)
Pain that disturbs your sleep despite regular medication
Stiffness that prevents you from putting on shoes or socks
Pain not adequately controlled by physiotherapy, injections, or tablets
X-ray evidence of significant joint damage
Reduced walking distance affecting your independence
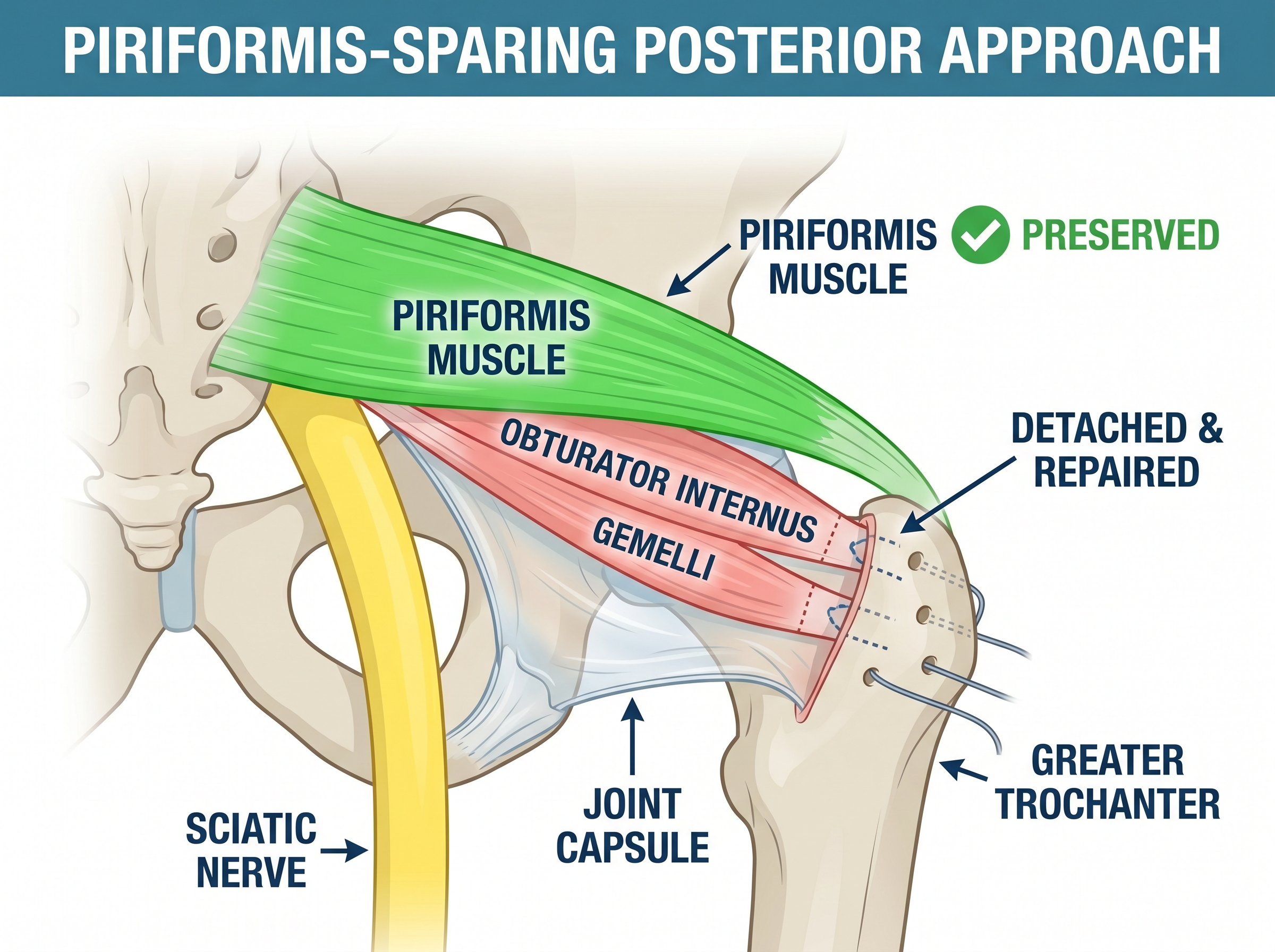
The Surgical Technique — Piriformis-Sparing Approach
Mr Dehne uses a modified posterior approach that preserves the piriformis muscle — the primary dynamic stabiliser of the hip. This technique provides the excellent surgical exposure of the traditional posterior approach while maintaining the stability benefits of muscle-sparing surgery.
What Makes This Technique Different
In a traditional posterior approach, the piriformis tendon is cut to access the hip joint. Mr Dehne's technique works around the piriformis, entering the joint through the interval between the piriformis and the short external rotators below it. This creates a "triple-layer" stability construct:
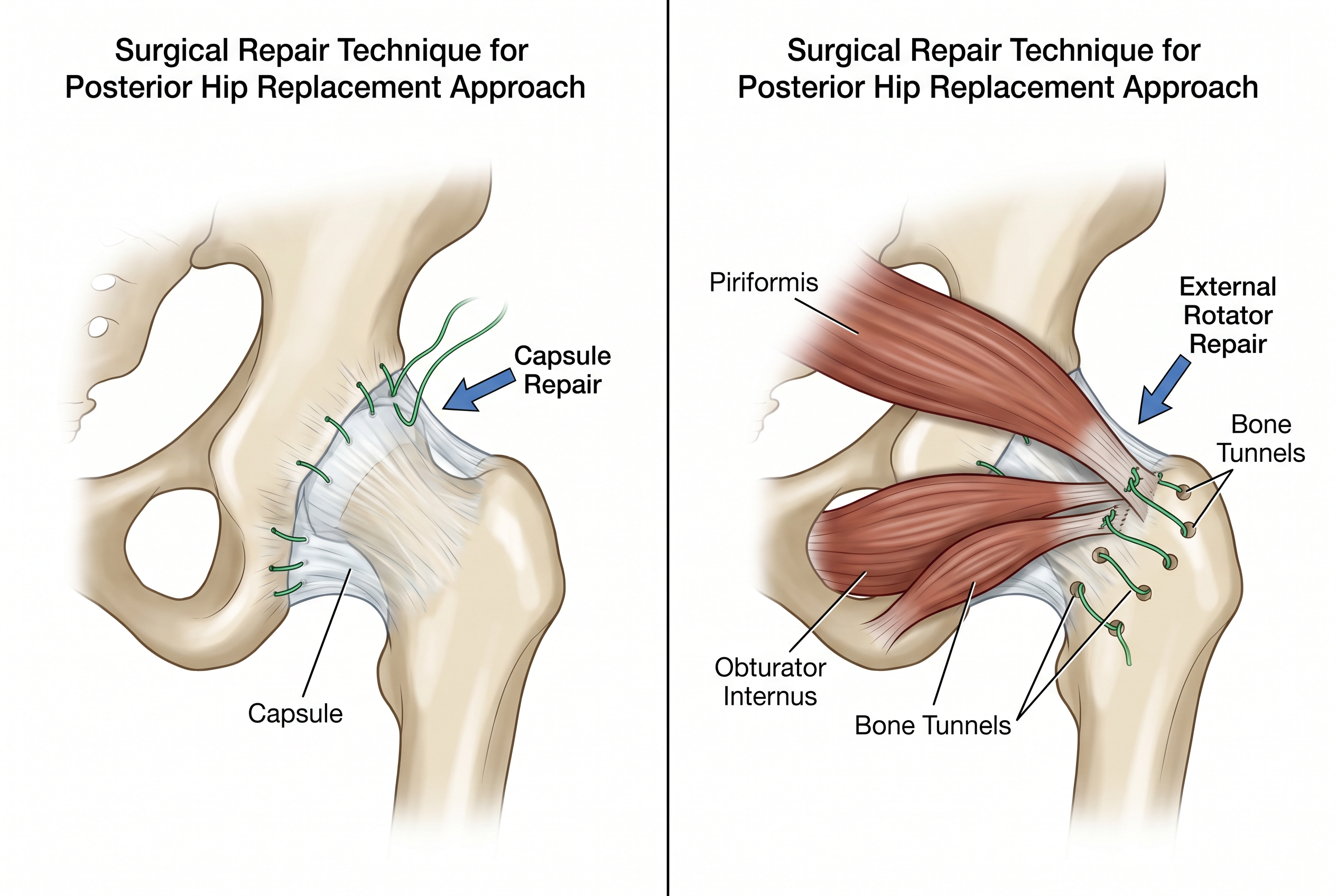
Layer 1: Preserved piriformis — The primary dynamic stabiliser remains intact and functional from day one
Layer 2: Repaired posterior capsule — The joint capsule is meticulously repaired back to bone using suture anchors
Layer 3: Repaired short external rotators — The remaining rotators are repaired over the capsule, creating a double-layer closure
The Surgical Steps
| Step | Description |
|---|---|
| 1. Incision | A 10–15cm incision on the back of the hip, following the line of the femur |
| 2. Muscle splitting | The gluteus maximus is split along its fibres (not cut), preserving its function |
| 3. Piriformis identification | The piriformis is identified and carefully retracted — NOT divided |
| 4. Capsulotomy | The joint capsule is opened below the piriformis with a planned repair in mind |
| 5. Femoral preparation | The damaged femoral head is removed and the canal prepared for the stem |
| 6. Acetabular preparation | The socket is reamed and the cup implanted with or without screws |
| 7. Trial reduction | Trial components are inserted to check leg length, stability, and range of motion |
| 8. Final implantation | Definitive components are implanted and the hip is reduced |
| 9. Triple-layer closure | Capsule repaired to bone, rotators repaired over capsule, piriformis confirmed intact |
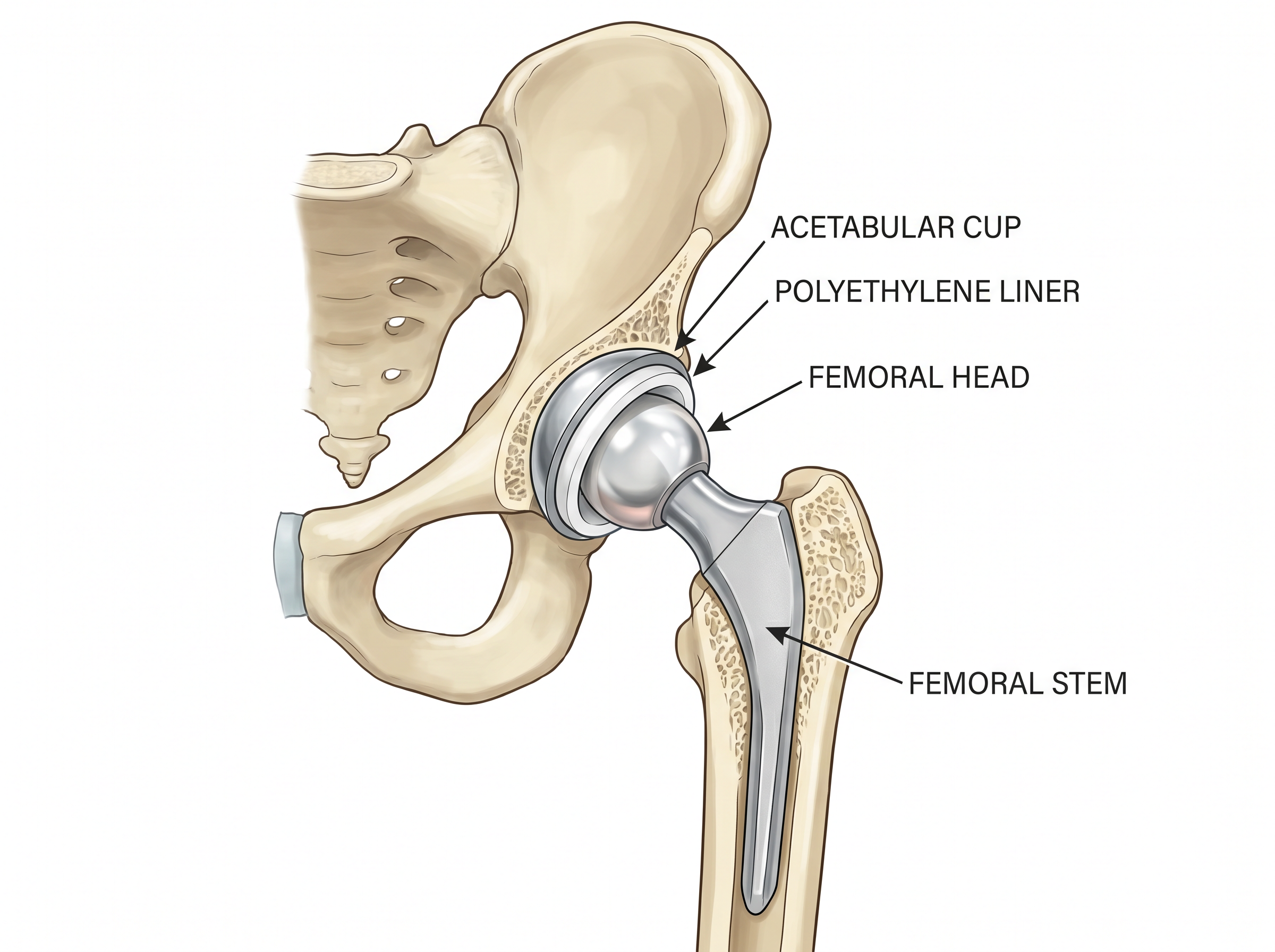
The Hip Replacement Components
A total hip replacement consists of four components that work together to recreate the natural ball-and-socket joint:
| Component | Material | Function |
|---|---|---|
| Acetabular cup | Titanium shell | Replaces the worn socket; press-fit into the pelvis |
| Liner | Highly cross-linked polyethylene or ceramic | Low-friction bearing surface inside the cup |
| Femoral head | Ceramic or cobalt-chrome | Replaces the ball; articulates with the liner |
| Femoral stem | Titanium alloy | Inserted into the femoral canal; supports the head |
The Evidence — Why This Approach Works
| Finding | Evidence |
|---|---|
| Reduced dislocation rate | Piriformis-sparing approach reduces dislocation risk to <0.5% compared to 2–3% with standard posterior approach |
| Faster recovery | Preserved piriformis allows earlier mobilisation and faster return to normal gait pattern |
| Better stability | Triple-layer repair provides stability comparable to anterior approach without the associated complications |
| Preserved function | External rotation strength preserved from day one — important for turning, pivoting, and balance |
| Excellent long-term outcomes | Over 95% of modern hip replacements last 15+ years; 90% still functioning well at 20 years |
Fast Recovery Programme
Mr Dehne's hip replacement programme is designed around the principles of Enhanced Recovery After Surgery (ERAS). The goal is to get you mobile, comfortable, and home as quickly and safely as possible.
| Timeline | Milestone |
|---|---|
| Day 0 (surgery day) | Up and walking with physiotherapist within 4–6 hours of surgery |
| Day 1 | Walking with frame/crutches, stairs practice, discharge criteria assessment |
| Day 1–2 | Most patients discharged home (some suitable for same-day discharge) |
| Week 2 | Wound check, walking with one crutch, driving assessment (automatic, left hip) |
| Week 6 | Follow-up with Mr Dehne, X-ray review, driving for all patients, return to desk work |
| 3 months | Return to physical work, most sports, unrestricted daily activities |
| 6 months | Full recovery, maximum improvement in function and pain relief |
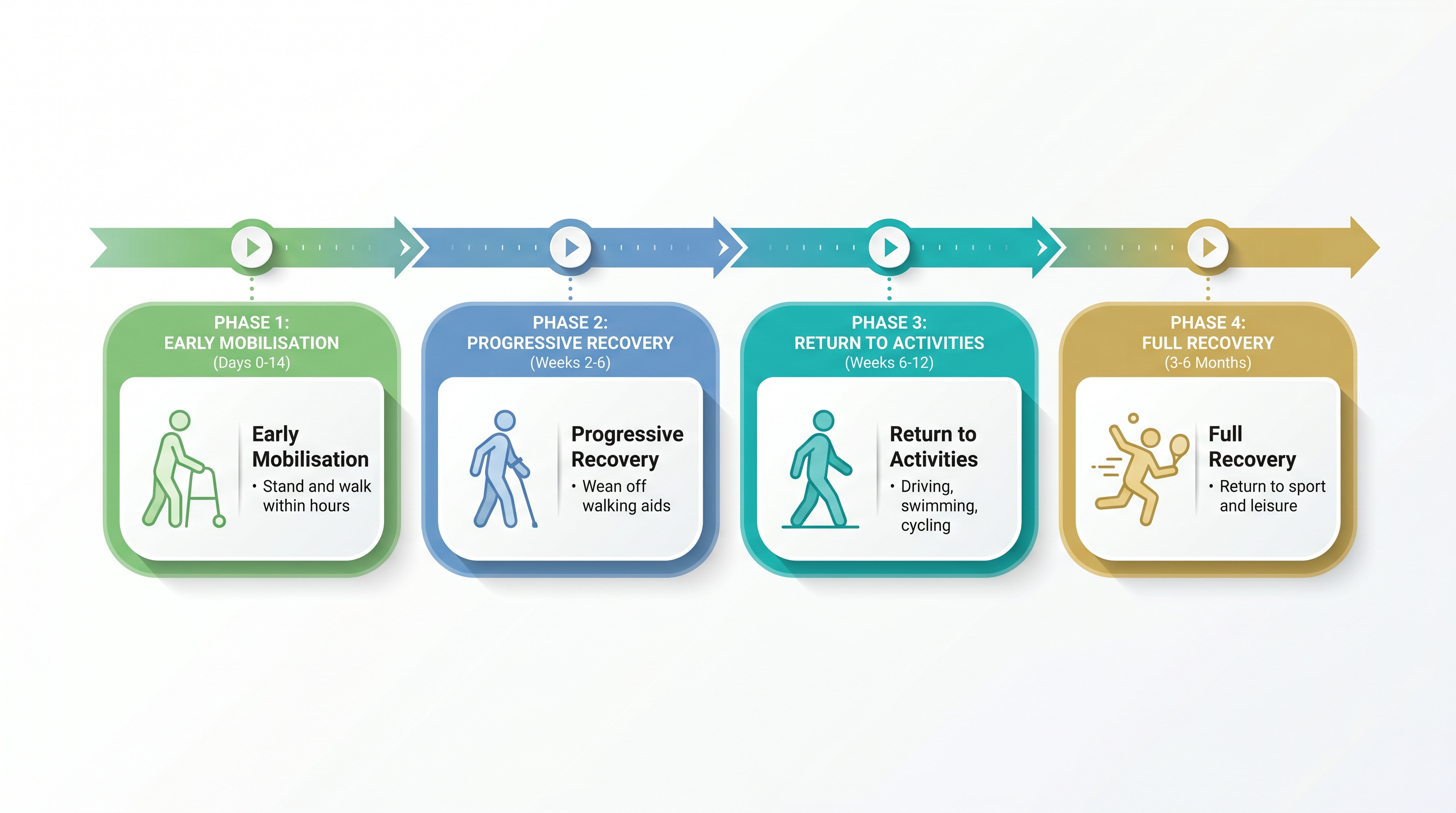
Rehabilitation Programme
Phase 1: Early Mobilisation (Days 0–14)
Weight bearing as tolerated with walking aids, restore basic mobility (bed transfers, toilet, stairs), gentle range of motion exercises, ankle pumps for DVT prevention, ice and elevation for swelling
Phase 2: Progressive Recovery (Weeks 2–6)
Wean from crutches to single stick, normalise walking pattern, increase hip range of motion, begin strengthening (bridging, standing hip exercises, mini squats), return to light daily activities
Phase 3: Return to Activities (Weeks 6–12)
Full weight bearing without aids, return to driving, swimming and cycling from 6 weeks, progressive strengthening and endurance, normal daily activities without restriction
Phase 4: Full Recovery (3–6 Months)
Return to sport (low-impact), full strength and endurance, no functional limitations, maximum improvement in Oxford Hip Score
Risks and Complications
Hip replacement is one of the most successful operations in modern medicine, with over 95% of patients reporting significant improvement in pain and function. However, like all surgery, it carries some risks.
| Complication | Frequency | Notes |
|---|---|---|
| Dislocation | < 0.5% (piriformis-sparing) | Significantly lower than standard posterior approach (2–3%) |
| Infection | < 1% | Antibiotics given during surgery; meticulous wound care |
| Blood clot (DVT/PE) | 1–2% | Blood thinners for 28 days post-op; early mobilisation |
| Leg length difference | Rare | Intra-operative assessment and templating minimise this risk |
| Nerve injury | < 0.5% | Usually temporary numbness; permanent injury very rare |
| Fracture | < 1% | Intra-operative fracture of femur or pelvis; managed at time of surgery |
Frequently Asked Questions
How long does the operation take?
The surgery typically takes 60–90 minutes. You will be in the operating theatre for approximately 2 hours including anaesthetic preparation and recovery.
How long will I stay in hospital?
Most patients go home on Day 1 or Day 2 after surgery. Some patients are suitable for same-day discharge. Your length of stay depends on meeting the functional discharge criteria, not a fixed timeframe.
When can I drive?
You can usually return to driving at 6 weeks, once you can safely perform an emergency stop. This will be confirmed at your follow-up appointment.
When can I return to work?
For desk-based work, most patients return at 4–6 weeks. For physical or manual work, 3 months is typical. Mr Dehne will advise based on your specific job requirements.
How long will my new hip last?
Modern hip replacements are designed to last 20–25 years or more. Over 90% of hip replacements are still functioning well at 15 years. Factors affecting longevity include activity level, body weight, and implant type.
Can I kneel or squat?
Yes, once fully recovered (usually 3–6 months). The triple-layer stability (preserved piriformis + repaired capsule + repaired rotators) provides excellent stability, and most patients regain a full range of movement.
Can I play sport?
Low-impact sports such as swimming, cycling, golf, walking, and doubles tennis are encouraged. High-impact activities (running, football, rugby) are generally discouraged as they may accelerate wear of the bearing surfaces.
Will I set off airport security?
Yes, metal implants will trigger airport metal detectors. You will be given a medical card confirming your hip replacement. Simply inform security staff.
Warning Signs — When to Seek Urgent Help
Contact Mr Dehne's team or attend A&E immediately if you experience:
Sudden severe pain in the calf or leg swelling (possible DVT)
Chest pain or sudden breathlessness (possible pulmonary embolism)
Increasing redness, warmth, or discharge from the wound (possible infection)
Fever above 38°C lasting more than 24 hours
Feeling that the hip has 'popped out' or sudden inability to weight bear
Numbness or weakness in the foot that does not resolve
References
- Siguier T, et al. Mini-incision anterior approach does not increase dislocation rate: a study of 1037 total hip replacements. Clin Orthop Relat Res. 2004;426:164-173.
- Pellicci PM, et al. Posterior approach to total hip replacement using enhanced posterior soft tissue repair. Clin Orthop Relat Res. 1998;355:224-228.
- Kwon MS, et al. Does the piriformis-sparing approach reduce dislocation risk? A systematic review. J Arthroplasty. 2006;21(6 Suppl 2):53-58.
- National Joint Registry (NJR). 20th Annual Report. 2023.
- Learmonth ID, et al. The operation of the century: total hip replacement. Lancet. 2007;370(9597):1508-1519.
- Kehlet H, Thienpont E. Fast-track hip and knee arthroplasty. Clin Orthop Relat Res. 2013;471(11):3596-3600.