Greater Trochanteric Pain Syndrome
Understanding lateral hip pain — causes, diagnosis, and evidence-based treatment options
Understanding Your Hip — Anatomy
The hip joint is one of the largest and most stable joints in the body. It is a ball-and-socket joint formed by the femoral head (ball) sitting within the acetabulum (socket) of the pelvis. While most people are familiar with the hip joint itself, the outer aspect of the hip — the lateral hip — is equally important and is the area affected in Greater Trochanteric Pain Syndrome.
The Greater Trochanter
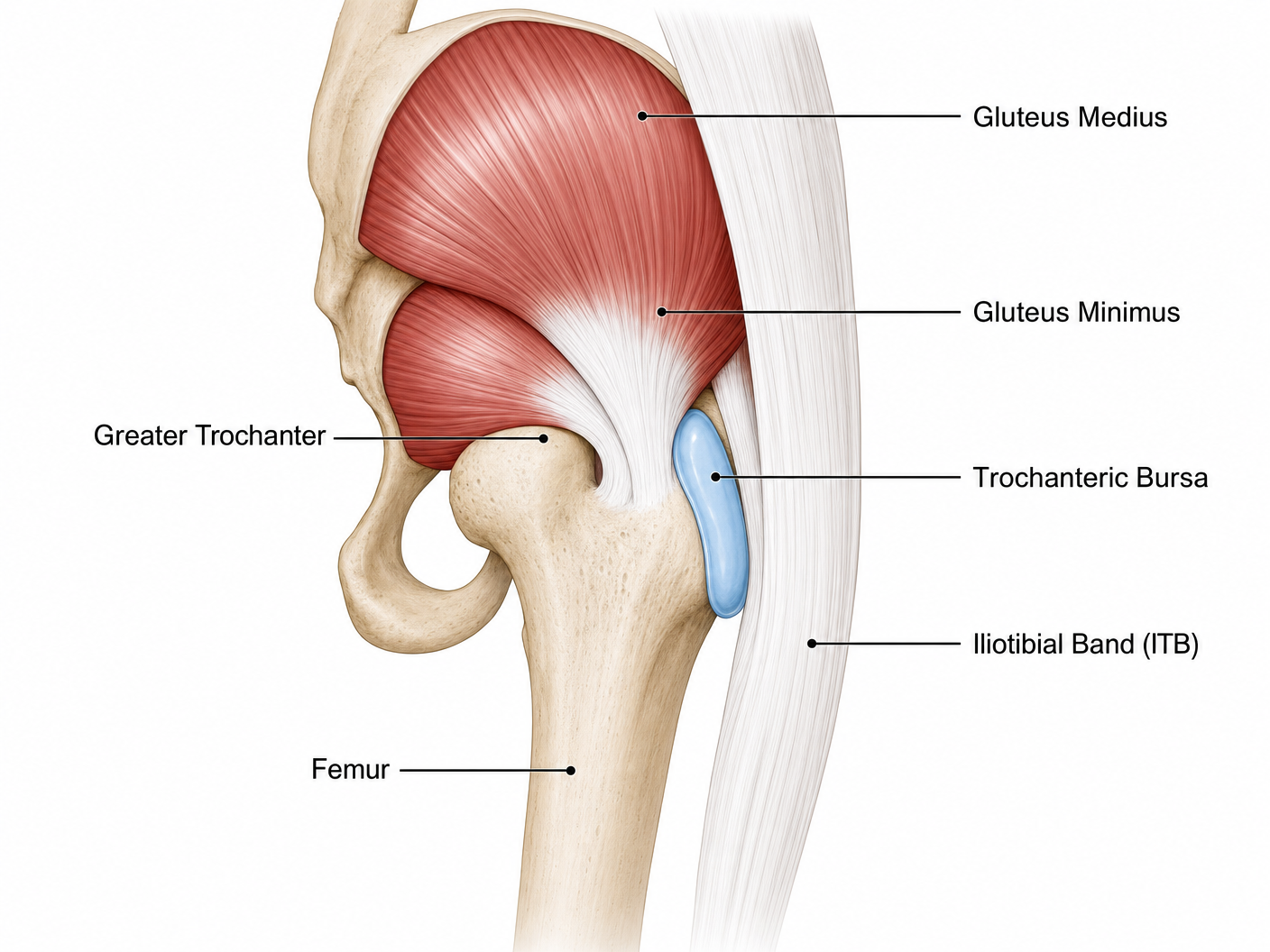
The greater trochanter is the bony prominence you can feel on the outer side of your hip. It is the attachment point for several important muscles and tendons that control hip movement and stability:
Gluteus medius — the primary hip abductor muscle that lifts your leg sideways and stabilises the pelvis during walking
Gluteus minimus — a deeper muscle that assists with hip abduction and internal rotation
Trochanteric bursa — a fluid-filled sac that reduces friction between the gluteal tendons and the iliotibial band (ITB)
Iliotibial band (ITB) — a thick band of connective tissue running from the pelvis down the outside of the thigh to the knee
What is Greater Trochanteric Pain Syndrome?
Greater Trochanteric Pain Syndrome (GTPS) is an umbrella term for conditions causing pain on the outer side of the hip, over or around the greater trochanter. It affects approximately 1.8 per 1,000 adults per year in primary care and is 2–3 times more common in women, typically presenting between the ages of 40 and 60.
| Condition | Description | Frequency |
|---|---|---|
| Gluteal tendinopathy | Degenerative changes in the gluteus medius and/or minimus tendons where they attach to the greater trochanter | Most common (60–70%) |
| Trochanteric bursitis | Inflammation of the trochanteric bursa between the gluteal tendons and the ITB | 15–20% |
| Gluteal tendon tears | Partial or complete tears of the gluteus medius or minimus tendons | 10–15% |
| External snapping hip | The ITB snapping over the greater trochanter during movement | 5–10% |
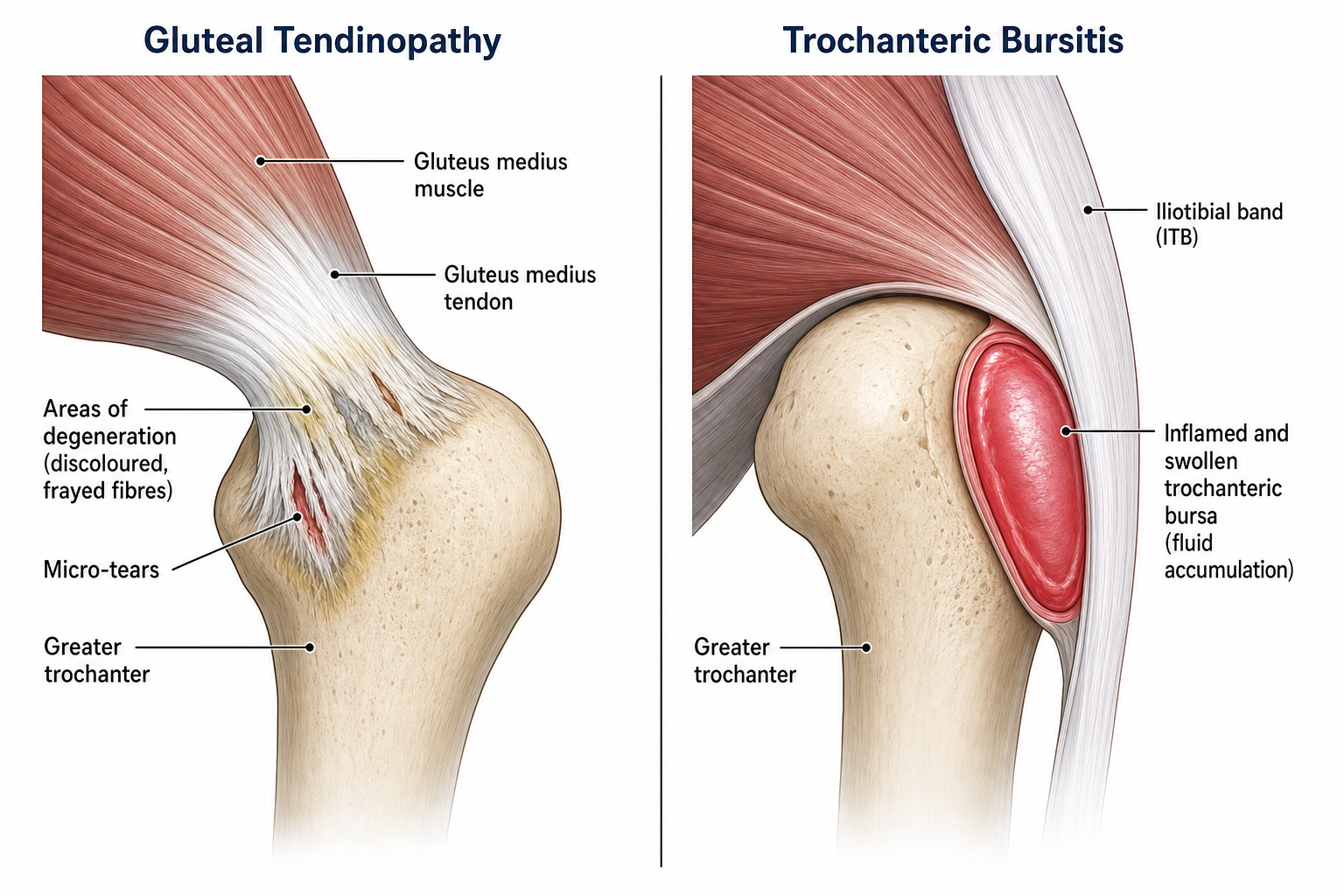
Previously, lateral hip pain was often labelled simply as 'trochanteric bursitis.' However, research using MRI and ultrasound has shown that isolated bursitis is actually quite rare — in most cases, the primary problem is gluteal tendinopathy (degeneration of the tendons), with bursitis being a secondary finding.
Causes and Risk Factors
| Category | Risk Factors |
|---|---|
| Biomechanical | Weak hip abductors, leg length discrepancy, wide pelvis (female anatomy), altered gait pattern, ITB tightness |
| Activity-related | Sudden increase in walking/running, prolonged standing, repetitive stair climbing, high-impact exercise |
| Postural | Habitual leg crossing, sleeping on affected side, standing with hip hitched, sitting on low chairs |
| Medical | Obesity (BMI > 25), lower back pain, osteoarthritis, previous hip surgery, hormonal changes (menopause) |
| Age & Gender | Women aged 40–60 most commonly affected (2–3× more common than in men) |
Signs and Symptoms
The hallmark symptom of GTPS is pain on the outer side of the hip. This pain typically:
Is localised over the bony prominence on the outside of your hip
Worsens when lying on the affected side at night
Increases with walking, climbing stairs, or prolonged standing
May radiate down the outer thigh (but not below the knee)
Is aggravated by crossing your legs or sitting in low chairs
May cause a limp during prolonged walking
| Severity | Typical Presentation |
|---|---|
| Mild | Pain only with specific activities (e.g., long walks, lying on side). Normal daily function. |
| Moderate | Pain with most weight-bearing activities. Disturbed sleep. Difficulty with stairs and prolonged standing. |
| Severe | Constant pain at rest and with activity. Significant sleep disturbance. Limp present. Unable to lie on either side. |
Diagnosis
GTPS is primarily diagnosed through clinical examination. Mr Dehne will assess your hip using specific tests:
| Test | What It Assesses |
|---|---|
| Palpation over greater trochanter | Direct tenderness at the tendon insertion |
| Resisted hip abduction | Pain/weakness suggesting gluteal tendinopathy |
| Single leg stance (30 seconds) | Pelvic drop indicating gluteal weakness |
| FABER test | Differentiates hip joint pathology from lateral pain |
| Trendelenburg test | Assesses gluteus medius function |
| Modified Ober's test | ITB tightness contributing to compression |
Imaging
Ultrasound (USS) is the first-line imaging modality — it can visualise tendon thickening, tears, bursal fluid, and guide injections in real-time. MRI may be requested for complex cases to assess the extent of tendon damage and rule out other pathology. X-rays are useful to exclude hip joint arthritis or calcification.
Treatment Options
Treatment follows a stepwise approach, starting with conservative measures and progressing if symptoms persist:
| Stage | Treatment | Expected Outcome |
|---|---|---|
| 1. Activity Modification | Avoid aggravating positions, sleep modifications, load management | Symptom reduction within 2–4 weeks |
| 2. Physiotherapy | Gluteal strengthening (isometric → isotonic → functional), ITB stretching, core stability | 60–70% improvement at 12 weeks |
| 3. USS-Guided Injection | Corticosteroid or PRP injection under ultrasound guidance | Significant pain relief for 3–12 months |
| 4. Shockwave Therapy | Extracorporeal shockwave therapy (ESWT) — 3–5 sessions | 68–79% success rate at 12 months |
| 5. Surgery | Gluteal tendon repair, bursectomy, or ITB release (rare) | Reserved for refractory cases (< 5% of patients) |
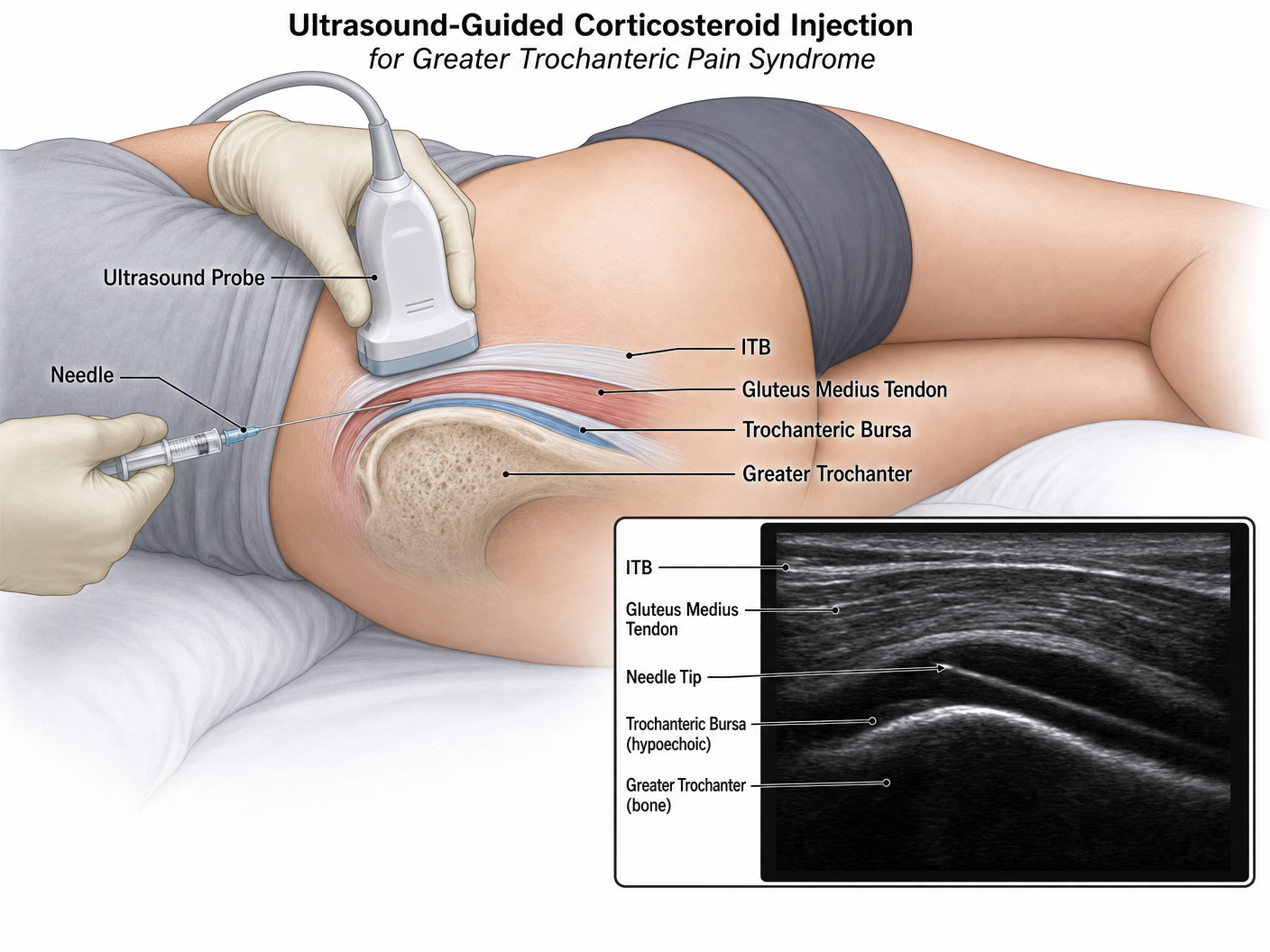
USS-Guided Injection Therapy
Ultrasound-guided injections allow precise delivery of medication directly to the affected area. Mr Dehne performs all injections under real-time ultrasound guidance to ensure accuracy and safety.
| Injection Type | Mechanism | Evidence |
|---|---|---|
| Corticosteroid | Reduces inflammation and pain rapidly. Best for acute flares and bursitis-predominant symptoms. | 75% pain relief at 4 weeks; effects may diminish by 3–6 months (Mellor et al., 2018) |
| PRP (Platelet-Rich Plasma) | Concentrated growth factors from your own blood to stimulate tendon healing. Better for chronic tendinopathy. | Superior long-term outcomes vs corticosteroid at 12 months (Fitzpatrick et al., 2019) |
After your injection: Avoid high-impact activity for 48 hours. You may experience temporary soreness at the injection site. Pain relief typically begins within 3–7 days for corticosteroid, and 4–6 weeks for PRP as healing occurs.
Extracorporeal Shockwave Therapy (ESWT)
Shockwave therapy uses focused acoustic waves to stimulate healing in damaged tendons. It is a non-invasive treatment option with strong evidence for GTPS:
Stimulates blood flow and neovascularisation in the damaged tendon
Triggers release of growth factors to promote tissue repair
Disrupts pain signalling and reduces chronic pain sensitisation
Breaks down calcific deposits if present
Protocol: Typically 3–5 sessions at weekly intervals. Each session lasts 10–15 minutes. Evidence shows 68% success rate at 4 months (Rompe et al., 2009) and 79% success at 12 months (Furia et al., 2009), with outcomes superior to corticosteroid injection at long-term follow-up.
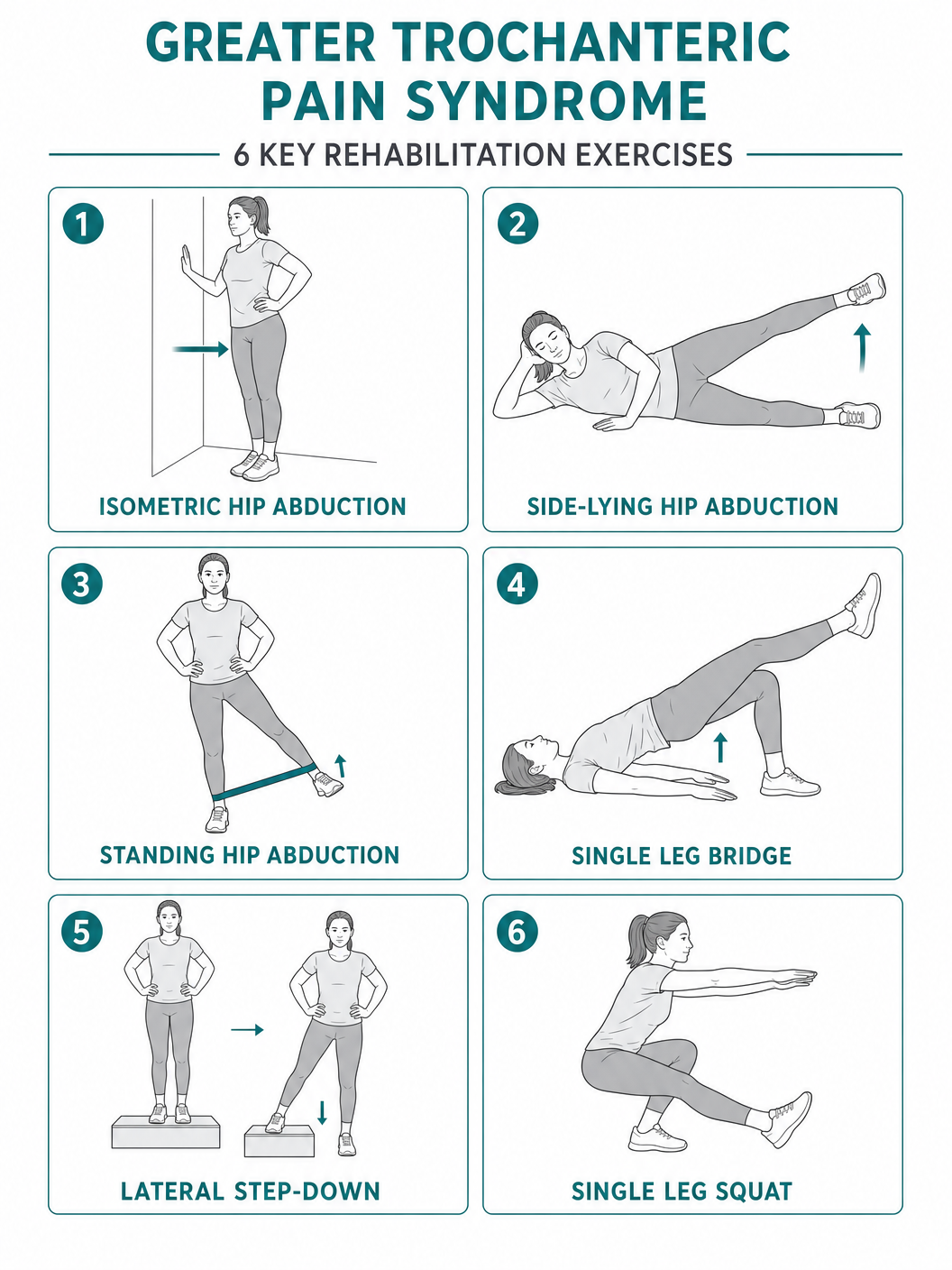
Rehabilitation Programme
Structured rehabilitation is the cornerstone of GTPS treatment. The programme follows a progressive loading approach through four phases:
Phase 1: Pain Management & Load Reduction
Weeks 0–2
Isometric gluteal holds (pain-free), gentle hip flexor stretches, sleep position modification (pillow between knees), avoid aggravating activities (crossing legs, standing on one leg)
Phase 2: Isometric Strengthening
Weeks 2–6
Side-lying isometric abduction (hold 30–45 sec × 5 reps, 3×/day), standing wall press (hip abduction against wall), bridging with band, core activation exercises
Phase 3: Isotonic Strengthening
Weeks 6–12
Side-lying hip abduction (progressive resistance), standing hip abduction with band, single-leg mini squats, step-ups (low step progressing to higher), clamshells with resistance band
Phase 4: Functional Rehabilitation
Weeks 12+
Single-leg balance and proprioception, lateral band walks, step-downs, sport-specific drills, gradual return to impact activities (walking → jogging → running)
Living with GTPS — Practical Advice
| Activity | Advice |
|---|---|
| Sleeping | Sleep on your back or unaffected side with a pillow between your knees. Use a mattress topper for pressure relief. |
| Sitting | Avoid low chairs and crossing your legs. Use a cushion for hard seats. Stand up and move every 30 minutes. |
| Walking | Maintain a normal stride length. Use a walking stick in the opposite hand if needed. Build distance gradually. |
| Stairs | Lead with the unaffected leg going up, affected leg going down. Use the handrail for support. |
| Driving | Use a cushion if the seat is low. Avoid long journeys without breaks. Swing both legs out together when exiting. |
| Exercise | Swimming and cycling are excellent low-impact options. Avoid running and high-impact activities until Phase 4 of rehabilitation. |
Frequently Asked Questions
How long does GTPS take to resolve?
With appropriate treatment, most patients see significant improvement within 3–6 months. However, some cases can take up to 12 months for full resolution. Early intervention and adherence to rehabilitation give the best outcomes.
Will I need surgery?
The vast majority of GTPS cases (over 95%) resolve with non-operative treatment. Surgery is only considered after at least 6–12 months of failed conservative management.
Can I still exercise?
Yes — but you need to modify your activities. Low-impact exercise (swimming, cycling, walking within pain limits) is encouraged. Avoid running, jumping, and activities that aggravate your symptoms until your physiotherapist advises progression.
Is GTPS the same as hip arthritis?
No. GTPS affects the tendons and bursa on the outside of the hip, while arthritis affects the hip joint itself (inside the groin). However, the two conditions can coexist, and Mr Dehne will differentiate between them during your assessment.
How many injections can I have?
Corticosteroid injections are typically limited to 2–3 per year to avoid tendon weakening. PRP injections do not carry this limitation and can be repeated if clinically indicated.
Why is it worse at night?
Lying on the affected side compresses the inflamed tendons and bursa against the bone. Even lying on the opposite side can stretch the ITB over the trochanter. Sleeping on your back with a pillow under your knees is usually most comfortable.
Warning Signs — When to Seek Urgent Help
While GTPS is not a dangerous condition, seek medical attention if you experience:
Sudden severe pain following a fall or trauma
Inability to bear weight on the affected leg
Redness, warmth, or swelling over the hip (possible infection)
Fever or feeling generally unwell alongside hip pain
Numbness or tingling extending below the knee
Rapid unexplained weight loss with hip pain
References
- Mellor R, et al. Education plus exercise versus corticosteroid injection for gluteal tendinopathy: a randomised clinical trial. BMJ. 2018;361:k1662.
- Fitzpatrick J, et al. The effectiveness of platelet-rich plasma injections in gluteal tendinopathy. Am J Sports Med. 2019;47(5):1130–1137.
- Rompe JD, et al. Home training, local corticosteroid injection, or radial shock wave therapy for greater trochanter pain syndrome. Am J Sports Med. 2009;37(10):1981–1990.
- Furia JP, et al. Low-energy extracorporeal shock wave therapy for greater trochanteric pain syndrome. Am J Sports Med. 2009;37(9):1806–1813.
- Grimaldi A, Fearon A. Gluteal tendinopathy: integrating pathomechanics and clinical features in its management. J Orthop Sports Phys Ther. 2015;45(11):910–922.
- Ganderton C, et al. Gluteal loading versus sham exercises to improve pain and dysfunction in postmenopausal women with greater trochanteric pain syndrome. J Women's Health. 2018;27(6):815–822.
- Ladurner A, et al. Management of greater trochanteric pain syndrome: a narrative review. Cureus. 2024;16(7):e65279.